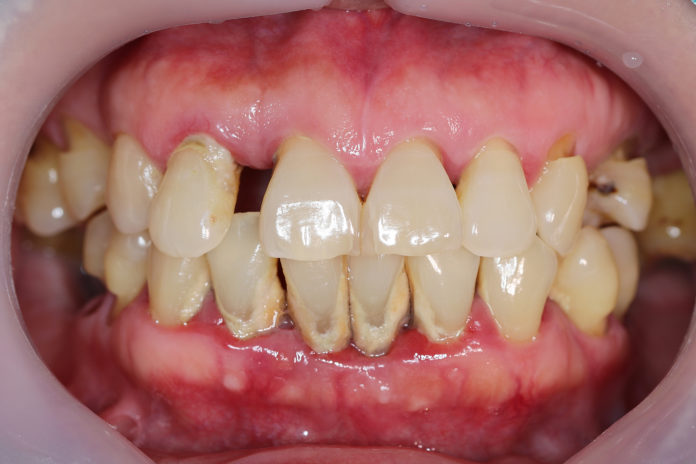
What is Periodontitis?
Periodontitis means inflammation surrounding the gum area. This is a common yet serious gum disease that progressively deteriorates the soft tissues around the teeth; this loosens the tooth structure and ultimately results in tooth loss.
Accumulation of bacteria around the teeth results in the formation of a transparent membrane around the teeth called plaque which if not removed will lead to hard calcification and tartar formation.
What are the symptoms of periodontitis?
Healthy teeth have firm, pale pink gums. Early stages of periodontitis have no or minuscule symptoms, but as the disease progresses, the following symptoms occur :
- Recurring swelling of gums
- Gingivitis
- Bleeding after brushing teeth
- Permanent bad breath, a condition called halitosis
- Reddish and bleeding gums
- Pus accumulation in between teeth and gums
- Pain while chewing
- Loosened teeth
- Receding gums giving the tooth an abnormally longer look
- Spaces in between teeth
- Tooth x-ray showing pocket development in between teeth and gums
Gingivitis is mostly painless; hence, patients tend to ignore these painless bleeding symptoms; on the contrary, these are the primary symptoms of growing periodontitis.
What are the causes of periodontitis?
You need to look out for the causes of periodontitis to take necessary precautions:
- Formation of plaque on your teeth: The moment sugars and other particles from the food you eat combine with the oral bacterial flora (already present in your mouth), plaque accumulates quickly over your teeth. However, if you brush your teeth twice daily and floss at least once, you can get rid of plaque.
- Plaque can lead to the formation of tartar: If you do not take proper care of your teeth and let plaque sit on them, it is likely to settle under your gumline and become calculus or tartar. As tartar is hard, it is tough to remove, and it also contains bacteria. The longer these stay on your teeth, the more damage they are likely to do. Once hardened, regular brushing and flossing cannot help you get rid of them, and you need to seek a professional dental cleaning service.
- Plaque can lead to gingivitis: Gingivitis is a gum disease that causes inflammation and discomfort to your gingiva (a portion of your gum near the base of your teeth). This gum condition is curable with proper oral care and dental treatment.
- Gum inflammation: If you have gum inflammation, it can be a cause of periodontitis. Prolonged inflammation in your gums creates gaps between your teeth and gum. These gaps eventually become home to tartar, plaque, and bacteria. With time, these gaps grow deeper and lead to infection. Gum inflammation, if left untreated, can damage your teeth and lead to teeth loss. This entire thing and put your immune system at stake, as well.
What are the risk factors of periodontitis?
Mentioned below are a few risk factors associated with periodontitis:
- Gingivitis (a gum disease)
- Improper oral habits
- Chewing tobacco
- Smoking
- Hormonal imbalance owing to menopause or pregnancy
- Consuming recreational drugs, including marijuana
- Vaping
- Being obese
- Heredity
- Malnutrition, such as Vit. C deficiency
- Having medications that may lead to dry mouth and changes in your gums
- Health conditions that suppress immunity, including HIV/AIDS, leukemia
- Other medical conditions, including Crohn’s disease, diabetes, and rheumatoid arthritis
- Cancer treatment
What are the complications associated with periodontitis?
Periodontitis causes tooth decay and ultimately, falling of teeth. Moreover, it has also been associated with increased CRP (C-reactive protein) levels and interleukin-6 proteins. This increases the risk of heart problems like atherosclerosis, myocardial infarction, hypertension and even stroke.
The bacteria from the tooth can also infect the bloodstream of the patients, thereby affecting faraway sites. These, in turn, cause various medical conditions like rheumatoid arthritis, respiratory disorders, coronary artery problems, and sugar control in diabetes
When to See a Doctor?
Bleeding of gums is the primary sign of developing periodontitis. Regular dental checkups should be done as soon as swelling of gums, chewing problems, loose teeth are observed.
Call 1860-500-1066 to book an appointment
How is periodontitis diagnosed ?
To diagnose periodontitis, your dentist will examine your mouth to look for plaque deposition and tartar buildup. He/she will also check if or not your gums are easily bleeding.
Once the oral examination is complete, your dentist will measure the depth of pockets (gaps) between your teeth and gum with the help of a dental probe at multiple sites. In a healthy mouth, the dental pockets measure around 1 mm to 3 mm deep. However, pockets with a depth of more than 4 mm can be a sign of periodontitis. If your oral pockets grow deeper than 5 mm, it could become hard to clean them well.
Then, your dentist is likely to take dental X-rays to find out if there is bone loss in the sites where the pockets are deep.
What are the treatment options for periodontitis?
Non-surgical procedures
If you don’t have advanced-stage periodontitis, the treatments are more likely to be less invasive. It includes the following:
- Scaling: It is a procedure that removes germs and tartar from the surface of your teeth and under your gums.
- Root planing: It is another dental procedure that smoothens the surface of the roots while eliminating the chances of bacteria and tartar buildup in the future. It also kills bacterial byproducts that may lead to delayed healing, inflammation, and other dental issues.
- Medications: Your dentist may also prescribe oral or topical antibiotics to check bacterial infection.
Surgical procedures
If your periodontitis has advanced, your doctor is more likely to recommend the following treatment procedures:
Pocket reduction surgery (Flap surgery): During this surgery, your periodontist will make small cuts in your gum to lift back a portion of the gum tissue. It will expose the roots, making root planing and scaling easy and more effective. As in most cases, periodontitis leads to bone loss, your dentist is more likely to recontour the underlying bone before stitching your gum tissue back. After recovery, it will become easier to keep these areas clean and have good gum tissues.
Soft tissue grafts: Your gumline happens to recede following the loss of gum tissue. In such cases, your dentist is likely to reinforce the marred soft tissues. During this procedure, the dentist will remove a small portion of tissue from your palate (roof of your mouth) or a donor’s mouth and graft it to the affected area of your gum. Soft tissue grafts reduce the recession of the gum line to a great extent. And this also covers the exposed parts of the root while giving a pleasant appearance to your teeth.
Bone grafting: In case, the bone surrounding the root of your tooth is damaged or destroyed, your periodontist is likely to perform bone grafting. The graft is made up of tiny fragments of bones (your bone, donor’s bone, or synthetic bone). This procedure holds your tooth in place while preventing tooth loss. Plus, it also acts as a platform for natural bone regrowth.
Tissue-stimulating proteins: During this surgical procedure, your dentist applies a special gel on the root of the diseased tooth. The gel comprises the same type of proteins as needed for tooth enamel development. This gel also helps stimulate the growth of healthy tissue and bone.
Guided tissue regeneration: This procedure helps regrow the bacteria-infected and damaged bone.
Medications
Mostly slow-release medications are used for long term relief.
- Antiseptic chip, where a small gelatin particle filled with an antimicrobial agent like chlorhexidine, is inserted into the root pockets after planing.
- Antibiotic gel: Doxycycline gel, an antibiotic agent, is placed on the root pockets to decrease the pocket size.
- Antibiotic microspheres: Microscopic beads containing minocycline, an antibiotic, are put into the root pockets to minimize bacterial growth.
- Oral medications of antibiotic
What are the preventive measures for periodontitis?
Mentioned below are some required preventions:
1. Brushing twice daily or if possible, after every meal will help prevent periodontitis.
2. Flossing regularly.
3. Using a soft-bristled toothbrush and changing brush after every 3-4 months. Clean the toothbrush after every wash.
4. An electric toothbrush is more effective in removing plaque.
5. A mouthwash containing antibacterial agents like chlorhexidine is necessary to prevent bacterial growth.
6. Using a fluoride toothpaste to safeguard tooth enamel.
7. Using an interdental brush or pick or cleaner to clean more effectively. Floss helps clean small spaces while dental picks help cleaning bigger spaces.
8. Consult a professional dentist regularly for tooth cleaning and other tests.
9. Prohibit smoking or using tobacco in any form.
10. Home remedies like saltwater rinses, aloe vera, turmeric are useful.
Frequently Asked Questions (FAQs)
Can periodontitis be reversed?
No, it can’t be reversed. Periodontitis causes permanent damage to the tooth; it can only be controlled or the bacterial infection can be minimized, to prevent further damage.
Can salt rinses cure periodontitis?
It surely helps. Regular gargling with warm salt water removes hidden bacteria from tooth pockets.
Are tea bags helpful curing swollen gums?
Pressing moist tea bags onto the painful swollen gums do help to soothe the pain and inflammation temporarily.