Overview
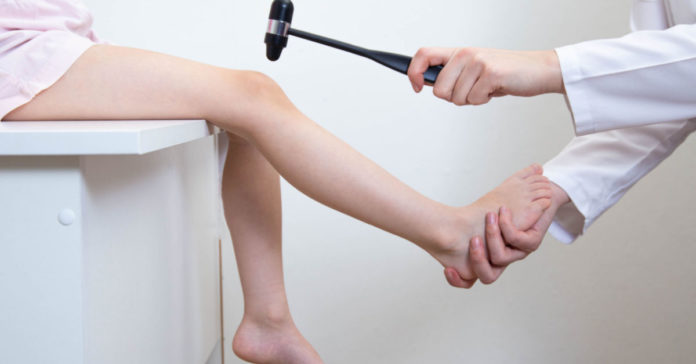
When a person gets a gentle tap on the knee, ankle, or fingers to elicit a reflex, but the tendons in those regions do not react to the stimuli and produce normal reflexes, it indicates a neurological disorder known as areflexia. Areflexia patients do not exhibit typical body reflexes, such as the knee-jerk reaction.
One of the leading causes of this disorder is nerve damage due to underlying health conditions. Genetics, spinal cord or brain injury, and alcohol abuse may lead to nerve damage. Based on the underlying cause of areflexia, the doctor determines and explains the various treatment and management options.
The blog explains areflexia, its symptoms, causes, and treatment options in detail.
What is areflexia?
A condition where a person’s deep tendon reflexes do not react to stimuli is known as areflexia. Tendons are tight cords of tissue that connect the muscles and bones and are responsible for the muscles to control and move involuntarily due to external stimuli. During a physical examination, the doctor gently taps on the side of the knee or ankle, and the leg involuntarily moves, a classic example of deep tendon reflexes. The arm, elbow, and abdomen also react similarly to external stimuli.
Reflexes are absent due to nerve damage in the muscle and tendons, injury to the spinal cord or brain, or underlying health conditions.
What is detrusor areflexia?
When the detrusor muscle fails to contract is known as detrusor areflexia. The bladder muscle helps and controls the bladder function, such as independently emptying the bladder. Detrusor areflexia happens when the detrusor muscle cannot contract. Detrusor muscle, a muscle in your bladder, controls emptying the bladder.
People with detrusor areflexia cannot empty their bladders on their own. They may need a hollow tube known as urinary catheter to release urine from your bladder. It is also known as an underactive bladder or neurogenic bladder. It is one of the symptoms of areflexia.
What are the symptoms of areflexia?
A complete absence of reflexes is the leading symptom of areflexia due to nerve damage. Other symptoms depend on underlying causes. However, other common symptoms may include the following:
- Tingling or numbness in the hands or feet
- Irregular muscle coordination
- Weakness in the muscle
- Lack of muscle coordination resulting in clumsiness and frequent dropping of things from hands or falling
- Lack of sexual desire, particularly in men
- Constipation
- Problems in digestion
- Detrusor areflexia
- Complete or partial paralysis
- Respiratory failure
- Loss of sensitivity to touch in fingers or toes
- Unexplained pain
When to seek medical advice?
Consulting a doctor immediately is advisable if a person experiences any of the symptoms.
What are the causes of areflexia?
The usual cause of an absent tendon reflex is peripheral neuropathy – a disorder in which a patient suffers a malfunction of the nerves due to damaged or destroyed nerves. In addition, a disease or an injury can also destroy or damage the nerves. Some of the disorders are listed below:
- Diabetes: Diabetic patients experience nerve damage due to uncontrolled sugar levels for prolonged periods, inflammation, and issues with the kidney and thyroid. Controlling blood sugar may reduce the chances of nerve damage.
- Vitamin deficiencies: The human body needs vitamins E, B1, B6, and B12 for nerve health. But when the body doesn’t receive the essential vitamins required for nerve health, it leads to areflexia.
- Guillain-Barre syndrome (GBS): In this disorder, the immune system attacks the healthy nerve cells in the peripheral nervous system. The cause of it is unknown, and many experts believe that an infection, such as stomach flu or Epstein-Barr virus, may have triggered it
- Miller fisher syndrome: It is a rare neurological disorder that the experts sometimes consider a subvariant of GBS. Similar to GBS, this is due to viral infection.
- Other autoimmune diseases: Multiple sclerosis, lupus, rheumatoid arthritis, or amyotrophic lateral sclerosis are some of the autoimmune diseases that result in nerve and tissue damage. Such conditions also cause weak or absent reflexes. For example, in multiple sclerosis patients, the immune system attacks and damages the protective layers of the nerve fibres, causing inflammation, injury, and scar tissue in the nervous system.
- Hypothyroidism: Here, the body produces low levels of thyroid hormones, causing fluid retention and increased nerve tissue pressure.
- Other organ-related diseases: Illnesses that affect the internal organs, such as kidney disease, liver disease, connective tissue disorder, and underactive thyroid, may lead to nerve damage .
- Infections: Certain viral or bacterial infections may result in neuropathic pain that affects reflexes. Infections such as Lyme disease, shingles, hepatitis B and C, and HIV are all linked to neuropathy.
- Medications: Prescription medications for severe health conditions and chemotherapy for cancer may have side effects, such as nerve damage.
- Tumours: Benign or cancerous tumours have the potential to affect nerves around them. The increased pressure from the tumours presses on the nerve, causing nerve damage.
- Nerve and spinal cord injury: Car accidents or falls are common causes of physical trauma and nerve injury. A spinal injury typically results in total loss of sensation and mobility below the injury site, including areflexia.
- Toxins and alcohol abuse: Constant exposure to toxic chemicals or heavy metals, such as lead or mercury, results in nerve damage. Alcoholics are at a higher risk of developing peripheral neuropathy.
The following are some of the rare disorders that cause areflexia:
- Chronic inflammatory demyelinating polyneuropathy (CIDP): This long-term condition destroys the brain’s nerve fibres, eventually leading to the loss of muscle reflexes. It is similar to GBS.
- Cerebellar ataxia, neuropathy, and vestibular areflexia (CANVAS) syndrome: This genetic, slow-progressive neurological disorder leads to gradual loss of coordination, areflexia, and other impairments. A person above 60 years typically develops this disorder.
- Cerebellar ataxia, areflexia, pes cavus, optic atrophy, and sensorineural hearing loss (CAPOS) syndrome: It is a rare hereditary disease that affects young children between the ages of 6 months and five years. It develops after an illness with a high fever. With the onset of CAPOS, the child may suddenly experience a lack of coordination and walking ability. Muscle weakness, hearing loss, swallowing issues, unusual eye movements, and areflexia are other symptoms of CAPOS. It is important to note that certain symptoms may improve once the fever is cured.
What are the various treatment options?
Based on the underlying cause, the doctor chooses a treatment plan for each patient. Sometimes, treating the health condition may help improve the symptoms. Other times the damage could be permanent, and treatment may help manage the pain. The healthcare provider may recommend medications that may help pain management; physical therapy may assist in muscle strengthening of the damaged nerve, or both.
- Medications: The doctor may prescribe medications for the cause of the symptoms. For example, diabetic patients get insulin to treat the disease, and GBS patients may be prescribed immunoglobulin therapy. Several medications may be used to treat autoimmune diseases.
- Physical therapy: The doctor teaches the patient to perform exercises to improve walking, running safely, and overall muscle strength. Such activities strengthen the affected muscles.
Currently, there are no medications to treat detrusor areflexia. The healthcare provider may suggest a urinary catheter to empty the bladder frequently. A thin, flexible tube, known as a catheter, is inserted into the patient’s bladder, which helps in urination.
Conclusion
Based on the underlying cause, the outlook for areflexia patients varies . Certain conditions, such as multiple sclerosis, are incurable. However, there are medications to manage the symptoms and improve the quality of life. Most Guillain-Barre syndrome patients make a complete recovery. The sooner the patient consults a doctor, the better chances of relieving the symptoms to lead an everyday life.
Frequently Asked Questions (FAQs):
How is areflexia preventable?
Certain conditions like injury, tumours, and autoimmune diseases are not under anyone’s control. However, other diseases, including liver diseases or type 2 diabetes, can be preventable by making healthy lifestyle choices, including a healthy diet and staying fit, thus helping the patient lower the risk of nerve damage.
What are the different ways doctors diagnose areflexia?
The doctor diagnoses areflexia by conducting the following tests:
- Blood test
- Spinal tap
- Nerve conduction study
- Electromyography
- CT scan or MRI