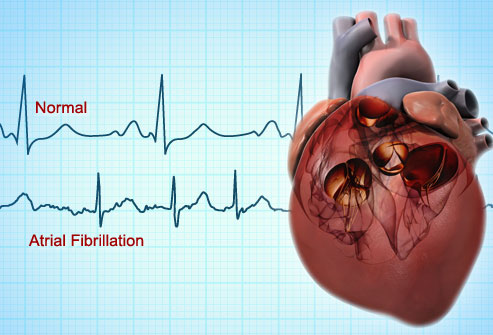
What is Atrial Fibrillation?
Atrial fibrillation is an irregular and chaotic rhythm (electrical disorder) that comes from the heart’s upper chambers. Normally, the heart’s upper two chambers generate electrical activity at 60-100 times a minute, but in atrial fibrillation patients, the upper chamber beats at 400-500 times per minute.
Luckily, ‘AV node’, the junction between the lower and upper chamber, allows only a few of those signals to reach the lower chamber. Despite this, the lower chambers still can beat as fast as 150-200 times per minute.
Overview
Incidents of atrial fibrillation can come and go, but if this health concern develops over time it may require medical attention. Though it is usually not a life-threatening condition, atrial fibrillation is still considered as a serious condition that may require emergency medical attention sometimes.
This condition may lead to complications and can cause the formation of blood clots in the heart that may circulate to other organs in the body. This eventually results in blocked blood flow (ischemia). Atrial fibrillation can be treated with medications along with other interventions to modify the electrical system of the heart.
What are the different types of Atrial Fibrillation?
Doctors have classified Atrial Fibrillation as following:
- Permanent: Afib happens when the condition continues for an unspecified period and, where the doctor along with the patient, decides to stop further treatment to bring back the real heart rhythm.
- Long-standing: This type of Afib is continuous and extends longer than 12 months
- Occasional or “Paroxysmal”: This occurs when your heart’s rhythm returns back to normal on its own within 7 days of its beginning. You may experience that symptoms may last for a few minutes to a few hours and then stops by itself.
- Persistent: In this type of Afib, your improper rhythm persists or continues for more than seven days and does not get back to normal on its own. If you suffer from persistent atrial fibrillation, you may require treatment like medications or an electrical shock to restore the rhythm of your heart.
Causes
The most common cause of atrial fibrillation is damage to the structure of the heart or abnormalities in it. Other possible causes of Afib include:
- High Blood Pressure
- Coronary Artery Disease
- Congenital heart disease
- Heart Surgery
- Heart Valve Disease
- Hypertrophic Cardiomyopathy
- An Overactive Thyroid Gland
- Taking Certain Medications
- Binge Drinking
- Thyroid Disease
- Pericarditis
- Heart attacks
- Abnormal heartbeat
- Sleep apnea
- Lung diseases
- Exposure to stimulants like alcohol, tobacco, caffeine or medications
- Viral infections
- Stress due to surgery, pneumonia or other illnesses
A healthy lifestyle may help reduce the chances of atrial fibrillation. However, not all causes are avoidable. It is very important to inform your medical practitioner about your medical history, so they can treat your condition better.
Symptoms
The faulty electrical signals make the heart beat faster than it should. The abnormal beating stops the heart from pumping enough blood. It can slow down enough to pool and form clots, which increases the risk of stroke and other heart issues. Along with fluttering and racing heart, a sharp throbbing pain and pressure in the chest may also be felt. Other symptoms include confusion, dizziness, and shortness of breath, sweating, tiredness, weakness and fatigue.
Where on the other hand, a few individuals with atrial fibrillation can show no signs of symptoms and are completely unaware of their heart condition. They only notice that there is a heart concern when it is found during a medical examination.
Those who do have this heart condition may experience symptoms like:
- Palpitations, which are uncomfortable, sensations of a racing, a flip-flopping in your chest or irregular heartbeat.
- Reduced ability to exercise
- Weakness
- Dizziness
- Confusion
- Shortness of breath
- Chest pain
- Fatigue
- Light-headedness
When To Consult a Doctor?
If you have observed any of the above symptoms, you must consult your medical practitioner immediately. Your doctor may order several tests and medical procedures to identify if your signs and symptoms are linked to the condition or any other arrhythmia treatments.
If you are suffering from chest pain, request for emergency medical support immediately. Chest pain is a sign that may be having a heart attack.
Complications
- Heart Failure: If left untreated, atrial fibrillation may weaken the heart and lead to heart failure.
- Stroke: The chaotic rhythm may cause blood to collect in the upper chambers of the heart thereby forming blood clots. If a blood clot forms, it could get dislodged from your heart and travel to the brain, blocking the blood flow thereby causing a stroke.
Also Read About: Blood Clot in The Brain
Diagnosis
To detect atrial fibrillation, your medical practitioner may asses your signs and symptoms, analyse your medical history, and perform a physical examination. In addition, your doctor may prescribe several tests to analyse your condition.
Here are some of the tests which help in assessing Atrial Fibrillation:
- Holter Monitor – Is a portable ECG device. It is worn on a shoulder strap, on a belt or can be carried in your pocket. It collects the data of your heart’s activity for 24 hours or longer. The information recorded by the device will provide your medical practitioner with an extended look at your heart rate.
- Electrocardiogram (ECG) – In this test, small sensors (electrodes) are used. They are attached to the arms and chest to detect and record electrical signals as they pass through the heart. ECG is the main tool for identifying atrial fibrillation.
- Blood Tests – A blood test assists your medical practitioner in ruling out any thyroid issues or other substances in your blood, which may cause atrial fibrillation.
- Chest X-Ray – X-ray pictures help your medical practitioner to see your lungs and your heart.
- Stress Test – It is also known as exercise testing and it involves running tests on your heart at the same time when you are exercising.
- Event Recorder – This is another portable ECG device and its primary goal is to observe your heart’s activity for a few weeks or months as suggested by your medical practitioner. You need to initiate this test only at the time when you are experiencing symptoms of a rapid heartbeat.
You just have to push a button when you are experiencing these symptoms and an ECG strip of the previous few minutes and next few minutes are recorded. This allows your medical practitioner to determine your heart rate at the exact time of the symptoms.
Treatment
The most appropriate treatment for atrial fibrillation will depend on how bothersome the symptoms are, duration of the condition and the basic cause of atrial fibrillation. The goal of the treatment is to prevent blood clots, reset the heart rate or rhythm and to minimize the risk of strokes.
The treatment plan that you and your medical practitioner choose depends on numerous factors, including whether if you are able to take heart rhythm controlling medicines and whether if you have other cardiac issues. In some cases, you may have to undergo invasive treatments.
In some individuals, a particular incident or an underlying health issue, such as a thyroid cancer, may give rise to atrial fibrillation. Treating the health issue causing atrial fibrillation may help relieve you from the heartbeat problems. If your signs and symptoms are troublesome or if this is your first incident of atrial fibrillation, your medical practitioner may try to reset the heart rate.
Prevention
To minimize your risk of developing atrial fibrillation, it is very important to maintain a heart-healthy lifestyle. Once you are diagnosed with the condition, you need to take medications as prescribed by your doctor. Also, you need to get appropriate treatment for your condition in order to minimize the harmful consequences of atrial fibrillation.
Here are some steps you need to take to prevent the condition from becoming worse:
- Eat a diet that is low in terms of cholesterol, saturated fats, Trans fats and salt
- Increase your physical exercise
- Quit smoking
- Maintain a healthy weight
- Avoid or limit your intake of alcohol and caffeine
- Reduce the amount of stress
- Manage your blood pressure levels
Risk Factors
Here are some of the most common risk factors of AFib:
- Age – As you get older, you are at greater risk of developing atrial fibrillation.
- Cardiac Disease – Any person with cardiac issues including congenital heart disease, heart valve problems, coronary artery disease, congestive heart failure, or a history of heart valve surgery or heart attack are at an increased risk of developing atrial fibrillation.
- High Blood Pressure – If you have high blood pressure and it’s not controlled well with medication or lifestyle changes, you are certainly at risk of developing atrial fibrillation.
- Other chronic conditions – Individuals with particular chronic ailments such as sleep apnea, thyroid cancer, diabetes, metabolic syndrome, interstitial lung disease or chronic kidney disease are at an increased risk of developing atrial fibrillation.
- Alcohol Consumption – For some individuals, consuming alcohol can cause an episode of atrial fibrillation. The risk increases with binge drinking.
- Obesity –Individuals who have obesity are at an increased risk of developing this heart condition.
- Family History – It is another risk factor that causes atrial fibrillation. If any of your family members had this condition, then you may also develop the same condition in the future.
Conclusion
The most important thing you can do to prevent atrial fibrillation is to adopt and live the healthiest life possible. You have to exercise regularly and take a heart-healthy checkup regularly to determine if you are at risk. Take a resolution today to slow down the aging process of your heart.