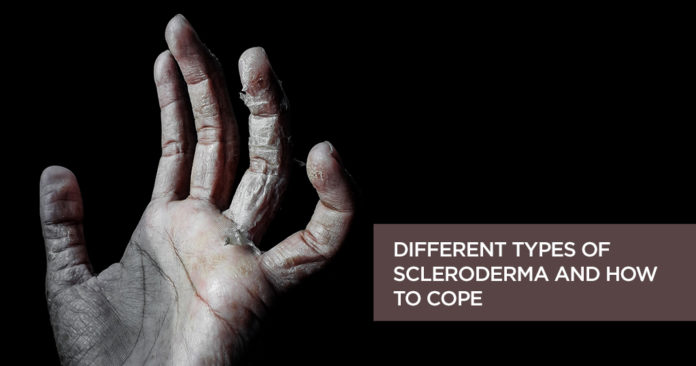
A scleroderma is a disease that hardens and tightens the skin and connective tissues. It is not a contagious (or infectious) disease. Women are at higher risk of getting scleroderma than men. Individuals between the ages of 35 and 50 are more prone to get scleroderma.
Although there is no cure for scleroderma, a variety of treatments can ease symptoms and improve the quality of life.
What causes Scleroderma?
Physicians are unsure of what causes scleroderma. This is among a category of disorders called autoimmune diseases. Collagen is an essential protein that helps in tightening of the skin. If our body’s immune system produces too much collagen, it results in scleroderma. As a result, our skin becomes tight and thick. This will result in scar formation on the lungs and kidneys. Blood vessels can thicken and cease to function. It results in the damage to the tissue and hypertension.
What are the types of Scleroderma?
There are several different types of Scleroderma. In some individuals, scleroderma affects only the skin. But in many people, Scleroderma also harms blood vessels, internal organs, and the digestive tract. This is called systemic Scleroderma.
Localized Scleroderma
It mainly affects the skin. It is of two types:-
Morphea:
The morphea form is a typical type of localized Scleroderma where there are oval shaped hard plaques on the skin with no presence of internal stiffening of tissue (sclerosis). They start out purple or red and later turn whitish in the centre. Sometimes, this type may affect internal organs or blood vessels. This known as generalized morphea.
Linear: This type lead to lines or streaks of thickened skin on your arms, legs, or face.
Systemic Scleroderma
Systemic Scleroderma can involve many body parts and is also known as generalized Scleroderma. It can be of two types:
Limited Scleroderma:
Limited Scleroderma affects the skin of the face, hands, and feet. It can damage the lungs, intestines, or esophagus. Limited Scleroderma is sometimes called CREST syndrome, after its five common signs:
● Calcinosis (accumulation of calcium nodules in the skin)
● Raynaud’s phenomenon (a disorder of blood vessels)
● Esophageal dysfunction
● Sclerodactyly (localized thickening and tightness of the skin of the fingers or toes.)
● Telangiectasia (small blood vessels grow near the surface of the skin)
Diffuse Scleroderma:
This type of Scleroderma affects the skin in the mid-body, upper arms, thighs, hands, and feet. The skin becomes thick. This damages the lungs, intestines, or esophagus.
What are the symptoms of scleroderma?
The signs and symptoms of scleroderma differ according to the affected part of the body:
1. Skin:
● Patches on the skin which are stiff and tight.
● Ovals or straight lines shaped patches.
● Patches cover larger areas of the torso and limbs.
● The shiny appearance of the skin.
● The affected area may have restrictions in movement.
● Lack of blood flow to parts of your body such as your fingers, toes, or nose, usually because of cold-causing Raynaud’s disease.
● The colour of your skin might turn red, white, or blue.
2. Digestive system:
● Heartburn or dysphagia, if the esophagus is affected.
● Cramps, bloating, diarrhea, or constipation, if the intestines are affected.
● Difficulty in absorbing nutrients due to improper function of intestinal muscles.
3. Heart, lungs, or kidneys:
The function of the vital organs like the lungs, heart, and kidneys can be affected by Scleroderma. The conditions can become critical if proper treatment is not carried out.
What are the risk factors associated with scleroderma?
The risk of developing Scleroderma depends upon several combined factors like-
● Genetics or history of Scleroderma in the family.
● Environmental triggers like certain viruses, medications, or drugs and repeated exposure to certain harmful substances or chemicals.
● Other autoimmune disorders like Rheumatoid Arthritis, Lupus, or Sjogren’s Syndrome
What are the complications of scleroderma?
The complications can range from mild to severe and can affect your:
● Fingertips:
The restricted blood flow leads to permanent damage to the tissue at the fingertips. In some cases, amputations of fingertips may be needed.
● Lungs:
The reduced lung function results in difficulty in breathing during exercise. High blood pressure in the arteries of the lungs is also a complication related to scleroderma.
● Kidneys:
The reduced kidney function leads to a rise in blood pressure and an increased protein level in your urine.
● Heart:
Abnormal heartbeats, congestive heart failure, and pressure on the right side of the heart are some of the cardiac complications of scleroderma.
● Teeth:
Smaller and narrower mouth, difficulty in brushing teeth, or to even have them professionally cleaned, abnormal production of saliva, and dental decay are some of the complications associated with scleroderma.
● Digestive system:
Scleroderma-related digestive problems can cause heartburn and difficulty swallowing. Often it may cause cramps, bloating, constipation, or diarrhea.
● Sexual function:
Erectile dysfunction in males and decreased sexual lubrication and constriction of the vaginal opening in the females are some complications.
How is scleroderma diagnosed?
It can be challenging to diagnose scleroderma. An inquiry about your health history and a physical examination is the first step a physician may carry to diagnose scleroderma. They might order tests including:
● Imaging tests such as X-rays and CT scans
● Blood tests
● Gastrointestinal tests
● Lung function tests
● Heart tests such as EKGs and echocardiograms
They might also take a small sample of skin (called a biopsy) for a specialist to look at under a microscope.
What are some medications to treat Scleroderma?
There is no cure for scleroderma. Drugs and therapies can control Scleroderma and make your life better. Your physician may suggest steroidal creams or pills to scale back the joint inflammation and pain, antihypertensive medications, medication to dilate blood vessels, immunosuppressants, Heartburn medication, Medications to help move food through your intestines, antibiotics and regular influenza or pneumonia vaccinations.
Pain management can be done with the help of your physical or occupational therapists. Therapy will improve strength and help to carry out daily tasks independently. Light and laser therapy may be used on the skin. Amputations and lung and other organ transplants are surgical methods that are considered as last resorts for treating scleroderma.
Patients are requested not to take medicines without consulting a registered physician. Please visit your nearest Apollo Hospital to get the correct diagnosis and treatment of Scleroderma.
Call 1860-500-1066 to book an appointment.
● You should avoid alcohol, caffeine, and free sugar like sweet carbonated drinks, and ice-creams from your diet.
● If you have or experience gastroesophageal reflux disorder, then please avoid citrus fruits, tomatoes, spicy and oily food from your diet.
Frequently Asked Questions (FAQs)
● Can Scleroderma go away?
There is no cure for Scleroderma at present. There have been cases where the skin complications associated with Scleroderma disappear on their own in two to five years. Generally, Scleroderma that attacks internal organs usually deteriorates with time.
● What is the life expectancy of a person with Scleroderma?
Many people do have a good prognosis for Scleroderma. They live a full productive life. However, some people who have Scleroderma in the heart, lungs, or kidney die because of organ dysfunction.
● Can you live everyday life with Scleroderma?
Yes, you can lead a near-normal life with Scleroderma. You have to be careful to avoid the cold. People who are more severely affected (e.g., those with Scleroderma affecting the lungs, or hand function limitations) are often restricted in what they can do.
● What tests confirm Scleroderma?
A routine complete blood count test is not sufficient to diagnose scleroderma. Many additional tests may be carried out depending on the clinical situation. A pulmonary function test may be done to measure the working condition of the lungs. CT chest scan may assess the extent to which the lung is involved. The physician might take an X-ray or take a small sample of the skin for laboratory testing.