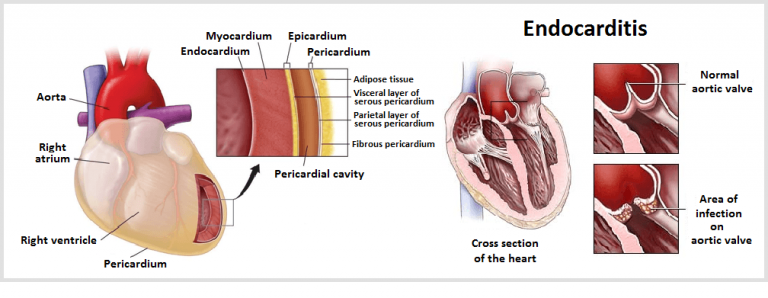
Endocarditis is termed as inflammation of the inner lining of the heart valves and heart chamber called endocardium. This condition usually occurs when fungi, bacteria or other germs from others parts of your body, such as the mouth, are spread through blood circulation and then attach themselves to the damaged regions in the heart. It can cause life-threatening complications by damaging your heart valves if it is not treated immediately. This condition can be treated by means of antibiotic medications and in some cases, surgery may be required.
Since there are numerous ways to develop this condition, your medical practitioner might not be able to identify the exact reason that caused endocarditis. However, individuals at higher risk of endocarditis generally have artificial heart valves, damaged heart valves, mitral valve repair or other heart ailments.
Endocarditis occurs when germs from other parts of the body enter the blood flow, reach the heart, and attach themselves to the damaged heart tissue or abnormal heart valves. In most cases, certain types of bacteria are the cause, while in some cases, fungi or other microorganisms may also cause this condition.
Generally, your immunity prevents dangerous bacteria from entering the bloodstream. Even if harmful, bacteria can make its way to the heart, they may pass through without triggering an infection. However, harmful bacteria that exists in your throat, mouth or any other part of your body like your gut or skin can at times cause serious infections like endocarditis.
Organisms that trigger endocarditis might enter your blood circulation through:
- A Medical Condition Or infection– Bacteria may pass from an infected region of the body, such as a skin sore. Apart from this, other medical issues like sexually transmitted infections, gum disease or certain intestinal ailments like inflammatory bowel disease can also provide bacteria a chance to enter your blood circulation.
- Everyday Oral Activities – Oral activities such as brushing your teeth daily may cause your gums to bleed. Gum bleeding enables bacteria to enter your bloodstream, especially if your gums and teeth are not healthy.
- Catheters – It is another way for bacteria to enter your body. A catheter is a thin tube that your medical practitioner uses it to remove fluid from the body. If the catheter is in place for a long period, then there is a higher chance for bacteria to enter the blood circulation.
- Illegal Intravenous (IV) Drug Use – Contaminated syringes and needles are a cause of concern for those individuals who use illegal intravenous (IV) drugs such as cocaine or heroin. People, who use these kinds of drugs repeatedly, do not have access to unused, clean syringes or needles.
- Needles Used For Body Piercing and Tattoos – The bacteria can also enter your blood circulation by means of needles used for body piercing or tattooing. This can also trigger endocarditis.
- Certain Dental Procedures – A few dental procedures may cause cuts in your gums, which allows bacteria to transmit through your bloodstream.
If the lining surface of your heart (endocardium) is rough, then bacteria can easily stick to the endocardium. If you have damaged, faulty or diseased heart valves, then you are at high risk of developing endocarditis.
Endocarditis Symptoms
Endocarditis may come up suddenly or slowly, based on the type of germs that are causing the infection, and depending on whether if you have any cardiac ailments. Endocarditis symptoms can differ from one person to another.
Here are some of the common symptoms of endocarditis:
- Fatigue
- A changed or new heart murmur, which is the heart sound made by blood passing through the heart
- Swelling in the legs, abdomen or feet
- Night sweats
- Bacterial endocarditis
- Aching muscles and joints
- Abnormal heartbeat
- Shortness of breath
- Flu-like symptoms like chills and fever
- Chest pain when you breathe
Endocarditis can also give rise to symptoms that are rare. These include:
- Unexplained weight loss.
- Softness in your spleen, which is an abdominal organ present on the left side of your body just under your rib cage that is key to immunity.
- Blood in urine, which you will be able to see or your doctor may find out when he/she analyses urine using a microscope.
- Jane way lesions, which are red spots on the palms of your hands or on soles of your feet.
- Osler’s nodes, which are red, tender spots under the skin of your toes or fingers.
- Petechial, which are red spots or tiny purple on the whites of your eyes, on the skin or inside your mouth?
There are several factors, which makes your doctor to suspect endocarditis. Diagnosis of endocarditis is generally based on numerous factors rather than a single symptom or a positive test result.
Your doctor may ask you to undergo several tests in order to make a positive diagnosis. These include:
- Blood Culture –This test is conducted to find out the presence of any fungi or bacteria in your bloodstream. It is perhaps the most important test your medical practitioner will conduct.
- Echocardiogram – It uses sound waves to generate images of your heart when it is beating. This test is generally used for checking signs of infection. In order to diagnose endocarditis, your doctor may use a transthoracic echocardiogram or transoesophageal echocardiograms.
- Transthoracic Echocardiogram – In this type of test, sound waves are aimed at your heart from the transducer (a wand like device) held on your chest to generate video images of your heart movements. This test enables your doctor to check for any signs of damage, or infection and also observe the structure of your heart.
- Transesophageal Echocardiogram – This is another type of echocardiogram that your doctors may conduct in order to get a closer look at your heart valves. This test can help your medical practitioners to get detailed images of your heart.
- Electrocardiogram (ECG) – This test is not particularly conducted to diagnose endocarditis. ECG can show your specialist if there is something affecting the electrical activity of your heart. While conducting an ECG, sensors are attached to your arms, legs, and chest. These sensors can detect your heart’s electrical activity. This test is performed to compute the duration and timing of each electrical phase in the heartbeat.
- Chest X-Ray – Using the images produced by the chest X-ray, your doctor will be able to view the condition of your heart and lungs. These images also help your doctor to see if endocarditis has caused any heart enlargement, or if there are any signs of any infection.
- MRI or CT scan – Depending upon the condition, your doctor may advise you to undergo an MRI or a CT scan of your chest, brain, or other parts of your body. It enables your doctor to analyse if the infection has spread to these areas.
In most cases, endocarditis is effectively treated by means of antibiotics. At times, surgery may be required to fix damaged heart valves and clean up any remaining signs of the infection.
-
Antibiotics
Doctors may recommend intravenous antibiotic therapy in case if your endocarditis is caused due to bacteria. You may have to take antibiotics until the time your infection is treated effectively. You will get these in a hospital for a minimum period one week until you show some signs of progress. Upon discharge from the hospital, you will have to continue antibiotic therapy as recommended by your doctor. Later on in your treatment, you may switch to oral antibiotics. Antibiotic therapy usually takes up to six weeks to complete.
-
Heart valve surgery
Damaged heart valves or prolonged infective endocarditis caused by endocarditis may require surgical treatment to correct. It is done to remove any scar tissue, dead tissue, debris or fluid build-up from infected tissue. The surgical procedure may also be required to remove or repair your damaged heart valve and substitute it with either animal tissue or man-made material.
Undergoing regular dental check-ups and maintaining good oral hygiene can help minimize the build-up of any bacteria in your mouth and prevent it from entering into your bloodstream. By doing this, you will be able to reduce your risk of developing endocarditis from an oral injury or infection. If you have gone through a dental treatment that was followed up with antibiotics, then ensure to take your medicines as prescribed.
If you have a history of heart surgery, congenital heart disease, or endocarditis, stay alert for the signs and symptoms of endocarditis. Take special care of unexplained fatigue or persistent fever.
you should also avoid:
- Illegal drug use
- Tattoos
- Body piercings
- Any unsterile procedure that may allow germs to get into your blood
Risk Factors
If you have a healthy heart, there is less chance for you to develop endocarditis, but it is still possible. The germs that trigger any infection have a tendency to stick to and proliferate on surgically implanted or damaged heart valves, or on endocardium that has a rough surface.
Individuals at greater risk of endocarditis are those who have:
- Congenital Heart Defects – Your heart may be more susceptible to infection if you were born with certain types of heart ailments like an abnormal heart valve or irregular heartbeat
- Artificial heart valves – There is a high possibility that germs will stick to an artificial (prosthetic) heart valve when compared to a normal heart valve.
- Damaged Heart Valves – Certain health issues like infection or rheumatic fever can harm or scar one or more of your heart valves. This can make them more susceptible to endocarditis.
- A History of Endocarditis – Endocarditis can damage heart valves or tissue that increases the risk of recurring heart infection.
- A History of Illegal Intravenous Drug Use – Those who inject illegal drugs are at higher risk of developing endocarditis. There is a high possibility that the needles used to inject illegal drugs can be contaminated with the bacteria.















