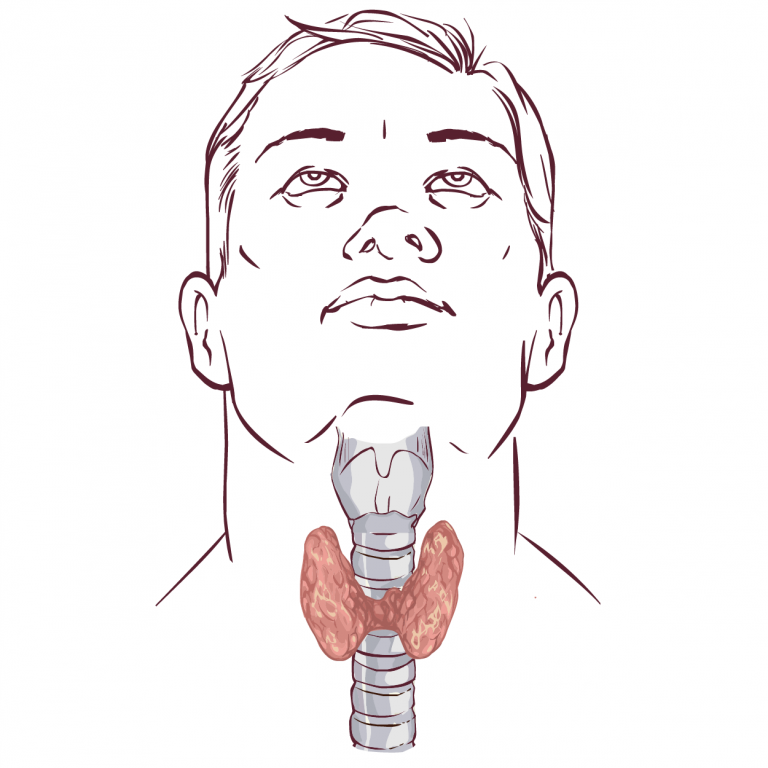
The thyroid gland produces thyroid hormones & it is situated below Adam’s apple in the lower part of the neck. The gland is present around the windpipe (trachea) & it has a shape similar to a butterfly – formed by two wings (lobes) & attached by a middle part (isthmus). The thyroid gland produces thyroid hormones by using iodine & most of it is available from the diet through foods like bread, seafood & salt. The two thyroid hormones that are produced by thyroid gland are thyroxine-tetra-iodothyronine or T4 & tri-iodothyronine or T3. T3 accounts for 1% & T4 accounts for 99% of thyroid hormones. Both are released into the blood after being secreted by the thyroid gland.
The most biologically active form of hormone is T3. Once T4 is released into the blood from the thyroid gland, T4 is converted into T3, & this active hormone affects the metabolism of cells. When thyroid hormone production slows down, the body’s processes also slow down & change. Hypothyroidism will affect various systems of the body.
Hypothyroidism or underactive thyroid is a condition in which the thyroid gland will not produce enough of thyroid hormones. Women, above 60 years of age, usually end up with hypothyroidism. Hypothyroidism causes an imbalance of chemical reactions in the body. If enough thyroid hormone is not produced in the bloodstream, the body’s metabolism slows down. Typical signs of an underactive thyroid are tiredness, weight gain & a feeling of depression. In the early stages, its symptoms are rare, but if left untreated, hypothyroidism leads to a number of health-related problems like heart disease, obesity, joint pain, infertility. It is a quite common condition affecting all age groups & races. However, women, especially older women are more prone to develop hypothyroidism than men.
Thyroid function tests help to diagnose hypothyroidism. Treatment with synthetic thyroid hormone is usually simple, safe & effective. There are no preventive measures for an underactive thyroid. An underactive thyroid is either caused due to the immune system attacking the thyroid gland & causing damage to it or by damage to the thyroid that occurs during some treatments for an overactive thyroid or thyroid cancer.
Both men & women can be affected by an underactive thyroid, but it is most common in women. In the western countries, it affects fifteen in every thousand women & one in a thousand men. Children can also develop an underactive thyroid. Around one in 3,500-4,000 babies are born with an underactive thyroid known as congenital hypothyroidism. The babies are screened for congenital hypothyroidism by taking blood spot test when the baby is about five days old.
The common causes of hypothyroidism are
- Hashimoto’s thyroiditis
- Thyroid destruction (from radioactive iodine or surgery)
- Lymphocytic thyroiditis (which may occur after hyperthyroidism)
- Medications
- Pituitary or hypothalamic disease
- Severe iodine deficiency
Hashimoto’s thyroiditis
An inherited condition known as Hashimoto’s thyroiditis is the most common cause of hypothyroidism. Dr. Hakaru Hashimoto described this condition in 1912 & is therefore named after him. In Hashimoto’s thyroiditis, the thyroid gland is enlarged goiter and the ability to make thyroid hormones is reduced. Hashimoto’s is an autoimmune disease in which the body’s immune system attacks the thyroid tissue. This condition is genetic & runs in families. Women are 5 to 10 times more affected when compared to men. The antibodies to the enzyme, thyroid peroxidase (anti-TPO antibodies) are increased in this condition.
Lymphocytic thyroiditis following hyperthyroidism
Inflammation of the thyroid gland is known as thyroiditis. As the inflammation is caused by a lymphocyte, a type of WBC cells, the condition is known as lymphocytic thyroiditis. It affects 8% of women after their delivery. In these patients, first, the hyperthyroid phase where excessive amounts of thyroid hormone are produced by the inflamed gland, followed by a hypothyroid phase that lasts up to six months. Most of the women return to normal state of normal thyroid function, but some remain in the hypothyroid state.
Thyroid destruction secondary to radioactive iodine or surgery
When hyperthyroid condition (such as Graves’ disease) patients receive radioactive iodine, they have very little of functional thyroid tissue after treatment.
The likelihood of this depends on some factors including the dose of iodine given, along with the size & the activity of the thyroid gland. If there is no significant activity of the thyroid gland six months after the radioactive iodine treatment, it is usually assumed that the thyroid will no longer function adequately. The result is hypothyroidism. Similarly, removal of the thyroid gland during surgery will be followed by hypothyroidism.
Hypothalamic or Pituitary disease
If for some reason the pituitary gland or the hypothalamus are unable to signal the thyroid & instruct it to produce thyroid hormones, a decreased level of circulating T4 & T3 may result, even if the thyroid gland itself is normal. If this defect is caused by pituitary disease, the condition is called “secondary hypothyroidism.” If the defect is due to hypothalamic disease, it is called “tertiary hypothyroidism.”
Pituitary injury
A pituitary injury may result from brain surgery or if there has been a decrease in blood supply to the area. In case of a pituitary injury, the TSH that is produced by the pituitary gland is deficient & blood levels of TSH are low. Hypothyroidism results because the thyroid gland is no longer stimulated by the pituitary TSH. This form of hypothyroidism can hence be distinguished from hypothyroidism that is caused by thyroid gland disease, in which the TSH level becomes elevated as the pituitary gland attempts to encourage thyroid hormone production by stimulating the thyroid gland with more TSH. Usually, hypothyroidism from pituitary gland injury occurs in conjunction with other hormone deficiencies, since the pituitary regulates other processes such as growth, reproduction, & adrenal function.
Medication
Medications which are used to treat an overactive thyroid may cause hypothyroidism. These drugs are Methimazole (Tapazole) & Propylthiouracil (PTU). The psychiatric medication, lithium (Eskalith, Lithobid), is also known to alter thyroid function & cause hypothyroidism. Interestingly, drugs containing a significant amount of iodine such as amiodarone (Cordarone), potassium iodide (SSKI, Pima), & Lugol’s solution can cause changes in thyroid function, which may result in low blood levels of thyroid hormone.
Severe iodine deficiency
Iodine deficiency in the diet causes severe hypothyroidism. It affects 5% to 15% of the population. It is seen in areas like India, Zaire, Chile, Ecuador. Severe iodine deficiency is also seen in mountain areas like the Himalayas & the Andes. Iodine deficiency is rarely seen in the United States due to the addition of iodine bread & table salt.
The signs & symptoms of hypothyroidism vary depending on the severity of the hormone deficiency. It will often take some years to develop hypothyroidism. At first, a person may barely notice the symptoms of hypothyroidism, such as fatigue & weight gain, or person may simply attribute them to getting older. But as the metabolism continues to slow down, more obvious signs & symptoms develop.
Signs & symptoms may include:
- Fatigue
- Increased sensitivity to cold
- Constipation
- Dry skin
- Weight gain
- Puffy face
- Hoarseness
- Muscle weakness
- Elevated blood cholesterol level
- Muscle aches, tenderness, and stiffness
- Pain, stiffness or swelling in your joints
- Heavier than normal/irregular menstrual periods
- Thinning of hair
- Slowed heart rate
- Depression
- Impaired memory
When hypothyroidism is not treated, signs & symptoms can gradually become more severe. Constant stimulation of the thyroid gland to release more hormones may lead to an enlarged thyroid (goiter). Also, the person may become more forgetful, thought processes may become slow, or a feeling of depression might arise.
Advanced hypothyroidism, also known as myxedema, is rare, but when it occurs, it can be life-threatening. Signs & symptoms include low blood pressure, decreased breathing, decreased body temperature, unresponsiveness & even coma. In extreme cases, myxedema can be fatal.
Hypothyroidism in infants
Although hypothyroidism most often affects middle-aged & older women, anyone can develop the condition, including infants. Initially, babies born without a thyroid gland or with a gland that doesn’t work properly may have few signs & symptoms. When newborns do have problems with hypothyroidism, they display the following issues:
- Yellowing of the skin & whites of the eyes (jaundice) – in most cases, this occurs when a baby’s liver cannot metabolize a substance called bilirubin, which usually forms when the body recycles old or damaged RBCs.
- Frequent choking
- A large & protruding tongue
- A puffy appearance to the face
As the disease progresses, infants are likely to have trouble feeding & may fail to grow & develop normally. They may also have:
- Constipation
- Poor muscle tone
- Excessive sleepiness
When hypothyroidism in infants is not treated, even mild cases can lead to severe physical & intellectual disabilities.
Hypothyroidism in children & teens
In general, children & teens who develop hypothyroidism have the same signs & symptoms as adults do, but they may also experience:
- Reduced growth, resulting in short stature
- Delayed development of permanent teeth
- Delayed puberty
- Poor mental development
Hypothyroidism can affect anyone, but increased risk is observed in:
- Women older than 60 of age
- Presence of autoimmune disease conditions
- The family history of thyroid disease
- Patients with rheumatoid arthritis or lupus, a chronic inflammatory condition
- Treatment with radioactive iodine or anti-thyroid medications
- Radiation to the neck or upper chest
- Have had thyroid surgery (partial thyroidectomy)
- Have been pregnant or delivered a baby within the past six months
Hypothyroidism can be suspected in patients with fatigue, cold intolerance, constipation & dry, flaky skin. A blood test is needed to confirm the diagnosis.
If hypothyroidism is present, the blood levels of thyroid hormones can be measured directly. They are usually found decreased. However, in early hypothyroidism, the level of thyroid hormones (T3 and T4) may be normal. Therefore, the main tool for the detection of hyperthyroidism is the measurement of the TSH, the thyroid-stimulating hormone. TSH is secreted by the pituitary gland and if a decrease in thyroid hormone happens, the pituitary gland reacts and produces more TSH & the blood TSH levels encourage production of thyroid hormone. This increase in TSH can precede the fall in thyroid hormones by months or years. Thus, the measurement of TSH should be elevated in cases of hypothyroidism.
However, an exception exists. If the decrease in thyroid hormone is actually due to a defect of the pituitary or hypothalamus, then the levels of TSH are abnormally low. As noted above, this kind of thyroid disease is known as “secondary” or “tertiary” hypothyroidism. A special test, known as the TRH test, can help distinguish if the disease is caused by a defect in the pituitary or the hypothalamus. This test requires an injection of the TRH hormone & is done by an endocrinologist (hormone specialist).
The blood work mentioned above confirms the diagnosis of hypothyroidism but does not point to an underlying cause. A combination of the patient’s clinical history, antibody screening & a thyroid scan can help diagnose underlying thyroid problem more precisely. If a pituitary or hypothalamic cause is suspected, an MRI of the brain & other studies may be done.
An underactive thyroid (hypothyroidism) is usually treated by taking daily hormone replacement tablets called levothyroxine. Levothyroxine replaces the thyroxine hormone when the thyroid does not make enough.
Initially, the patient will have regular blood tests to adjust the correct dose of levothyroxine. The patient is started with a low dose of levothyroxine, which would be increased gradually, depending on the patient’s body response. Some people begin to feel healthy soon after the beginning of treatment, while others do not notice an improvement in their symptoms for several months.
Once the patient takes the correct dose, he/she usually will have a blood test once a year to monitor the hormone levels.
If blood tests suggest an underactive thyroid, but no symptoms are noted, or only mild symptoms are seen, the patient may not need any treatment. In these cases, the general physician will usually investigate the hormone levels for every few months & prescribe levothyroxine if the patient develops symptoms.
Taking Levothyroxine
If the patient has prescribed levothyroxine, one tablet at the same time every day is usually taken. The patient usually takes the tablets in the morning, although some people prefer to take them at night.
The effectiveness of the tablets can be altered by other medications, supplements or foods, so they should be swallowed with water on an empty stomach, & should avoid eating for 30 minutes afterward. If the patient skips taking a dose, the dose should be taken as soon as the patient remembers.
An underactive thyroid is a lifelong condition, so the patient usually needs to take levothyroxine for the rest of the life.
Side Effects
Levothyroxine does not usually have any side effects because the tablets simply replace a missing hormone.
Side effects usually occur if the patient is taking too much levothyroxine. It can cause problems including headaches, sweating, chest pain, vomitings & diarrhea.
Combination Therapy
Combination therapy (using levothyroxine & triiodothyronine (T3) in combination) – It is not routinely used because there is insufficient evidence to show that it is better than using levothyroxine alone (monotherapy).
In most cases, suppressing thyroid-stimulating hormone (TSH) using high dose thyroid replacement therapy should be avoided because it carries a risk of causing adverse side effects, such as atrial fibrillation (irregular and abnormally fast heart rate), strokes, osteoporosis, & fracture.
However, this type of treatment may sometimes be suggested in cases where a person has a history of thyroid cancer & there’s a significant risk of it reoccurring.
Underactive thyroid & pregnancy
It is necessary to treat an underactive thyroid before pregnancy. If the patient is pregnant or trying to become pregnant & have hypothyroidism. They may refer to a specialist for treatment & monitoring during the pregnancy.
The common cause of hypothyroidism is Hashimoto’s thyroiditis, which cannot be prevented. Although hypothyroidism cannot be prevented, some symptoms of the disease need to be watched for, so that it can be treated properly. Some patients who are at high risk of having hypothyroidism but do not have symptoms can be tested to see whether they have mild, or subclinical, hypothyroidism.
- Stop smoking
- Exercise daily and maintain fit conditions
- Reduce stress
- Filtered water should be used for drinking, water containing fluoride will worsen the risk of thyroid problems.
- Iodine content consumed should be moderate otherwise it may lead to other health problems.
- Avoid foods containing excess fat















