Epilepsy is a neurological (central nervous system) disorder. In this, the cluster of nerve cells present in the brain gives abnormal signals, and the normal pattern of neuronal activity is affected. The brain activity becomes abnormal, causing periods of unusual behavior or seizures, muscle spasms, and sometimes, loss of awareness and sensations. A spectrum of brain disorders can cause epilepsies and seizures. They may be life-threatening sometimes.
If you have a single seizure, it does not mean that you have epilepsy. Epilepsy requires at least two unprovoked seizures. During an episode, some people may manifest twitching of arms and legs while some may have a blank stare. It affects both females and males of all races and ages.
Most people with seizures lead a normal, healthy life. In the epileptic patients, the two life-threatening conditions are status epilepticus and even sudden death (unexplained). In status epilepticus, the patients may have a prolonged seizure or they main not regain consciousness for a prolonged period after a seizure.
Epilepsy can be caused by an abnormality in the brain development or from a severe illness that may cause brain damage. Some disorders that may cause brain damage leading to epilepsy could be Alzheimer’s disease, head injury, pre-natal injuries and poisoning. Other causes that may trigger seizures are hormonal changes (during menstrual cycle or pregnancy), lack of good sleep, stress and alcohol consumption.
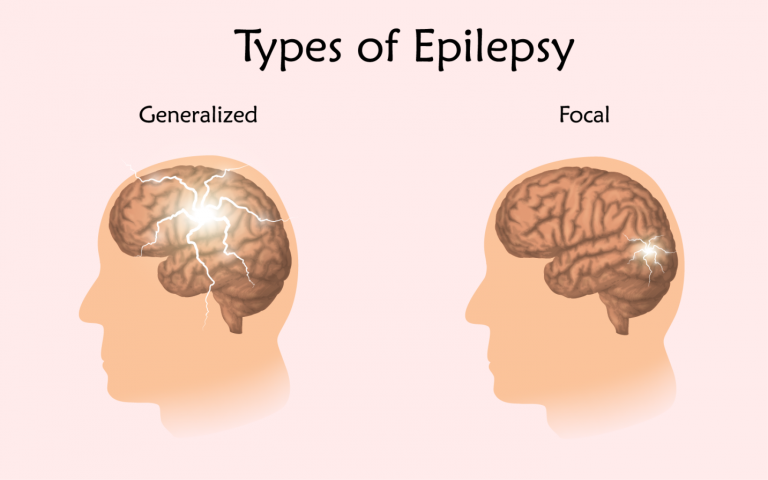
Seizures are divided into two major categories. They are focal and generalized seizures.
In a majority of the people who have epilepsy, dietary changes, medical management or occasionally surgical intervention is required. Some patients may need life-long treatment.
When a normal pattern of neuronal (nerves) activity is disturbed, it can cause seizures. Various reasons may cause disturbances in neuronal activity.
The major causes of epilepsy are
- Genetic factors
- Imbalance of neurotransmitters
- Illness-causing the brain damage (neurocysticercosis – a parasitic infection of the brain)
- Stroke
- Metabolic disorders (pyruvate dependency, tuberous sclerosis)
- Developmental disorders (cerebral palsy, neurofibromatosis, Landau-Kleffner syndrome, and autism)
- Changes in non-neuronal brain cells (known as glia)
- Prenatal injury causing problems
- Poisoning (exposure to poisons such as carbon monoxide and lead, overdose of anti-depressants)
- Infections (meningitis, viral encephalitis, AIDS and hydrocephalus (excess fluid is present in the brain)
- Trauma (head injury)
- Alzheimer’s disease
- Other causes such as brain tumors and chronic alcoholism, smoking, celiac disease (intolerance to wheat gluten) and
Neurotransmitters
- Epilepsy can also be caused by some inhibitory neurotransmitters such as GABA (gamma-aminobutyric acid), and research studies are going to find the effect of excitatory neurotransmitters such as glutamate. Some people with epilepsy have an abnormally high level of excitatory and abnormally low level of inhibitory neurotransmitters in the brain.
Genetic Factors
Sometimes some abnormal genes can cause epilepsy.
- Some defective genes that run in the families may cause epilepsy. Another gene codes for a protein called cystatin B is missing in people with progressive myoclonus epilepsy.
- LaFora’s disease ( a severe form of epilepsy) is caused due to alteration in another gene that causes breaking down of carbohydrates.
- Some abnormalities in the genes that control neuronal migration (an essential and critical step in brain development) can lead to abnormally formed neurons such as dysplasia in the brain which can trigger epilepsy.
- Some genes are sensitive to environmental factors and may also trigger seizures.
Prenatal Injury
- Epilepsy is caused by problems such as brain damage before birth. The infections in the mother during the pregnancy, oxygen deficiencies, poor oxygen may also trigger seizures and cause epilepsy.
Other Disorders
- Other disorders that may develop into epilepsy are brain tumors and stroke.Alzheimer’s disease and alcoholism may frequently lead to epilepsy. In most of the elderly people, epilepsy may cause a cerebrovascular disease. The reduction of oxygen supply to the brain causes epilepsy.
Other Causes
- Other causes that may trigger seizures are lack of sleep, smoking, hormonal imbalance, stroke, and alcohol consumption. They may provoke breakthrough seizures in people who have good seizure control with medications. In smoking, the nicotine present in the cigarettes acts on acetylcholine receptors (excitatory neurotransmitter) present in the brain.
The abnormal activity of the brain causes seizures. The signs and symptoms of seizures may vary depending on the type of seizure and may include:
- Involuntary movements (jerking) of the arms and legs (uncontrollable)
- Loss of awareness of surroundings or consciousness
- A blank staring spell
- Temporary loss of memory or confusion
- Other psychic symptoms such as fear, déjà vu (feeling that the current situation has already happened sometime in the past) or anxiety.
Certain important factors may increase the risk of epilepsy such as
- Family history: Increased risk of epilepsy is seen when you have family members with epilepsy.
- Age: The risk of epilepsy is most commonly seen in children and older adults. However, it can occur at any age.
- Trauma: Injuries to the head caused due to road traffic accidents (such as bicycling, skiing and motor vehicle accidents) may be responsible for few cases of epilepsy.
- Dementia: In older adults, dementia increases the risk of epilepsy.
- Infections: Infections of the brain such as meningitis or inflammations of the spinal cord can also increase the risk.
- Stroke and other vascular diseases: Stroke can trigger epilepsy and resultant brain damage is caused by other vascular disorders.
- Excessive intake of alcohol.
- Smoking cigarettes (due to nicotine).
- Seizures During Childhood: In a few patients, the seizures during childhood can be triggered by a high fever. These seizures may increase the risk if it is present for a long duration.
If you have a seizure or are predisposed to epilepsy, you have to consult your doctor immediately. Your doctor may ask you about your complete medical history and may also ask questions related to your exposure to epilepsy. The cause or triggering factors that are responsible for your seizures or epilepsy has to be identified first.
Complete neurological examination and neuropsychological tests: Your doctor may test your motor abilities, mental function and behavior to diagnose your condition. These tests help to determine the areas of your brain that are affected. Your memory, thinking, and speech skills are usually assessed. The type of epilepsy has to be determined before your treatment is initiated.
- Blood Samples: The signs of infections or genes that may be associated with seizures are identified with blood tests.
- Imaging: Some cases of epilepsy may be associated with areas of dysplasia in the brain occurring before birth and can be identified through advanced brain imaging.
- Computerized Tomography (CT) scan: Cross-sectional images of your brain are obtained using x-rays in a CT scan. The causes of your seizures are identified. Some causes could be tumors, cysts, and bleeding.
- Magnetic Resonance Imaging (MRI): A detailed view of your brain is observed in an MRI scan that uses radio waves and powerful magnets. Abnormalities of the brain or lesions in the brain that causes seizures can be identified.
- Functional MRI (fMRI): The exact locations of critical functions of the brain and changes in the flow of blood in the brain are identified (such as areas of movement and speech). It is usually done before the surgeries so that these places are not operated during surgical procedures of the brain.
- Electroencephalogram (EEG): It is the most common test used for the diagnosis of epilepsy. The doctors attach electrodes to your head with a paste-like substance. These electrodes help in recording the electrical activities of the brain. Your doctor may observe your response in a video to record any seizures that you may experience. These recordings help them to determine the kind of seizures you are having. It also helps in ruling out the other conditions causing epilepsy.
- High-density EEG: The electrodes are spaced more closely on the scalp (about half a centimeter apart from each other) compared to that of the conventional EEG. This determines the areas of the brain that are affected precisely and is helpful to determine the type of seizure.
- Advanced Imaging: Brain abnormalities can be detected using advanced tests such as:
- Positron Emission Tomography (PET): The active areas of the brain and the abnormalities of the brain are visualized. In this, low-dose radioactive material is injected into the vein of a patient.
- Single-Photon Emission Computerized Tomography (SPECT): SPECT identifies the pinpoint location in your brain responsible for seizures. It is done in patients when other diagnostic tests such as EEG and MRI are unable to locate the area. Low-dose radioactive material is injected into the vein of a patient and activity of the flow of blood during a seizure is noted.
- SISCOM (subtraction ictal SPECT coregistered to MRI): They provide the best diagnostic results in epileptic patients.
- Statistical Parametric Mapping (SPM): The different areas of the brain are compared during an episode of seizure and normal status in the patient. This helps in identifying the areas where the seizures have begun.
- Analysis Techniques: The pinpoint areas where the seizures start in the brain are identified.
- Curry Analysis: It is a technique that takes EEG data in a patient and projects it onto an MRI of the brain to observe the location of seizures.
- Magnetoencephalography (MEG): The potential areas of onset of the seizure is identified. MEG measures the magnetic fields that are produced by brain activity in the patient.
Treatment mostly includes medical management with anti-epileptic medicines. Surgery and other treatments are preferred if a patient does not respond to medical management.
1) Medical Management
Many factors are considered before the anti-epileptic medications are prescribed to patients such as age, the frequency of seizures and other factors. Most people with epilepsy, take one anti-epileptic medication and become seizure-free. While in other patients, a combination of drugs is used to decrease the intensity and frequency of the seizures. Anti-epileptic medications can be discontinued if the patient is seizure-free for 2-3 years on the advice of a doctor.
Most of the anti-epileptic medications have many side effects such as dizziness, weight gain, skin rashes, speech problems, loss of coordination, fatigue and memory and thinking problems. Suicidal thoughts and behaviors, severe rash and depression are some of the more severe side effects.
The below steps are followed to achieve the best seizure control possible with anti-epileptic medications:
- The prescribed medications must regularly be taken.
- Never overuse or stop the prescribed medicines, without consulting your doctor.
- When you observe unusual changes in your behavior or mood, suicidal thoughts and increased feelings of depression, then you must consult your doctor immediately.
- Herbal remedies, over-the-counter drugs, and other non-prescribed medications must not be taken without the consent of your doctor.
2) Surgery
Surgery is preferred in a patient if he does not have any good response to medical management. In surgery, the area of your brain that is responsible for seizures is removed. The surgery is only preferred in the following cases –
when the area that is operated does not interfere with vital functions like motor function, language, speech, hearing and vision, and
when seizures originate from a specific area of the brain.
3) Vagus Nerve Stimulation
This device can usually reduce seizures by 20 to 40 percent. The vagus nerve stimulator (an implant) is placed under the chest, and the stimulator is connected to the vagus nerve in your neck by wires. It inhibits seizures (reason not known) but may give rise many side effects, such as hoarse voice, shortness of breath, throat pain, or coughing from the vagus nerve stimulation.
4) Ketogenic Diet
In this diet, to obtain energy, the body breaks down fats instead of carbohydrates. Reduction in seizures was observed in a few children taking ketogenic diet under the close supervision of their doctors. Side effects include constipation, dehydration, slowed growth and kidney stones. Other foods that provide some benefit for seizure control are modified Atkins diets and low-glycemic index.
5) Many potential and new treatments for epilepsy are still being researched such as
- Deep Brain Stimulation: The electrodes are implanted into thalamus (specific area of your brain). The electrodes implanted in your chest are connected to a generator. They send electrical pulses to your brain.
- Responsive Neurostimulation: It is a pacemaker-like device that is Implantable. They analyze brain activity patterns to detect seizures. They detect seizures before they happen and stop them.
- Continuous Stimulation of the Seizure onset zone (subthreshold stimulation): Giving a continuous stimulation to an area of your brain below a physically noticeable level appears to improve seizure outcomes and quality of life of a person.
- Minimally Invasive Surgery: MRI-guided laser ablation, a new non-invasive technique shows promise of reducing seizures than traditional surgery.
- Radiosurgery or Stereotactic Laser Ablation: In patients where an open procedure may be too risky, radiosurgery or laser ablation may be the treatment of choice. The radiation of a specific area of the brain causing seizures is destroyed.
- External Nerve Stimulation Device: No surgery is required to implant this device. This device stimulates specific nerves to reduce the seizures.
1) Safety Measures
Head Injury can lead to seizures or epilepsy. Safety measures such as using helmets while riding a motorcycle or wearing seat belts in cars can protect people from head injury causing epilepsy.
2) Epilepsy Support Groups
They aid in better cope up of individuals affected with epilepsy.
3) Lifestyle and Home Remedies
Many lifestyle changes and remedies can be employed to prevent epilepsy such as:
- Good sleep: Adequate rest every night is important.
- Exercise: Regular exercising may help you to be physically fit and healthy.
- Taking your medication regularly
- Managing stress
- Limit the consumption of alcohol
- Avoid smoking
4) Education and Awareness
Educating yourself and your friends and family about epilepsy and its causes.
1) What is epilepsy?
Epilepsy is a disorder characterized by affected and disturbed nerve cell activities in the brain causing seizures.
2) What is the treatment provided for epilepsy?
In most patients (around 80%), epilepsy is treated with anti-epileptic medications that control seizures very well. However, in 20% patients, surgical management is preferred.
3) Can you suspect a seizure before it occurs?
The most well-known warning signs of a seizure are auras. You may also notice a peculiar taste in your mouth, an odd smell or experience a visual disturbance, such as seeing flashy lights and blurry vision. You may feel as though the temperature in the room has changed or hear a non-existent musical sound.
4) Can I die from an epileptic seizure?
Although death from an epileptic seizure is very rare, it is not uncommon. Respiratory or heart failure is often the culprits causing death in the patients due to SUDEP (Sudden unexpected death occurring during epilepsy), status epilepticus and other seizure-related causes.
5) What is the most dangerous type of seizure?
Generalized tonic-clonic seizures (grand mal seizures) are the most dangerous type of seizures. They are also known as convulsive seizures. These are the most frightening seizures to watch as the patient often becomes unresponsive.
Apollo Hospitals has the Best Neurologist in India. To find the best Neurologist doctors in your nearby city, visit the links below:















