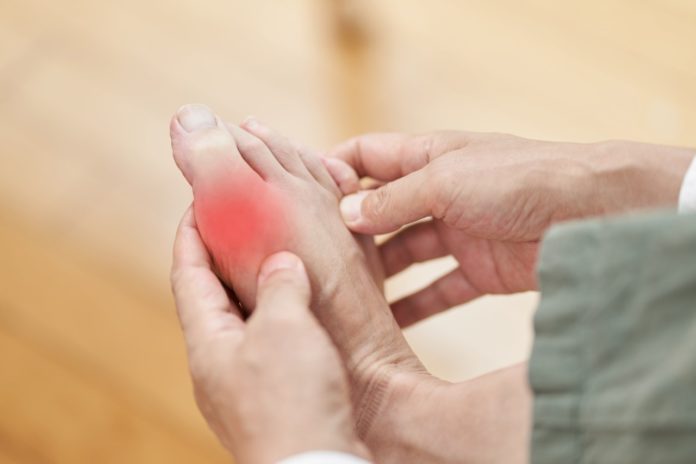
Hyperuricemia is a common condition in which there is an elevated level of uric acid in blood. Hyperuricemia occurs when your body either produces too much uric acid or is unable to excrete enough of it.
Causes
Causes of increased uric acid production
- Hereditary or genetic
- Consumption of purine-rich foods: Under physiological conditions, uric acid is produced in the body from the breakdown of certain carbon and nitrogen-containing compounds known as purines. Although purines are natural chemical components of our DNA and RNA, they are also present in high concentrations in certain foods such as meat, beans, seafood, sugary foods and beverages, and alcoholic beverages. Increased consumption of such purine-rich foods causes hyperuricemia over time
- Hematological disorders such as haemolytic anemia, leukemia, lymphoma
- Autoimmune conditions such as psoriasis
- Radiation and chemotherapy
- Obesity
- Unknown cause(s)
Causes of decreased uric acid excretion
- Kidney diseases: Uric acid is normally removed from the body by the kidneys. However, kidney diseases, including dysfunction caused by uncontrolled diabetes and hypertension, may decrease the kidneys’ efficiency of uric acid removal, leading to a rise in the uric acid levels in the blood.
- Certain drugs: like diuretics and immunosuppressant drugs
What are the symptoms of hyperuricemia?
Hyperuricemia is largely asymptomatic, with only approximately one-third of patients experiencing symptoms.
Symptomatic conditions which can result from hyperuricemia include:
Gout
Gout, sometimes called gouty arthritis, is an acute-onset, inflammatory arthritis which develops owing to hyperuricemia-induced formation of urate crystals, which tend to deposit in and around joint tissue. When the white blood cells attack and scavenge the crystals, it leads to the production of chemical mediators called cytokines which modulate inflammation, swelling and pain.
Gout can affect any joint in the body, occurring one joint at a time, with the feet, ankles, knees and elbows being common sites. The sudden “attacks” or “flares” commonly appear first in the large toe, often at night. Some triggers for gout attacks include joint injury, infection, surgical procedures, crash diets, rapid lowering of uric acid levels through medication, and dehydration.
If left untreated, acute gout can progress to chronic gout.
Gout Symptoms:
- Intense pain and swelling in affected joints, followed by periods of remission
- Redness and swelling of joints
- Joint stiffness
- Joint deformity
Tophaceous gout
Long-standing hyperuricemia can lead to the build-up and deposition of visible, and often disfiguring clumps under skin and around joints, called “tophi”. Tophi cause tendon and cartilage inflammation and bone erosion, and can aggravate joint pain.
Kidney stones
Long-standing hyperuricemia can also lead to formation of urate stones in the kidneys. Small stones can be excreted in the urine, however larger stones are difficult to eliminate and may block parts of the urinary tract.
Symptoms of kidney stones include:
- Pain in groin, lower back, or abdomen
- Nausea
- Increased urge to urine
- Painful urination
- Difficulty in urinating
- Blood in urine
- Foul smelling urine
- If urinary tract infection sets in, fever accompanied by chills, may be present
What are some risk factors for developing hyperuricemia?
Hyperuricemia could be due to a combination of hormonal, dietary or hereditary factors. In certain cases, drug therapy or certain medical conditions may also be responsible.
- Age and gender: Men between 30 to 50 years of age are more likely to have symptoms of gout. In women, the disease onset has most commonly been seen to be post-menopause. Gout is rare in children and younger adults.
- Family history: People with first-degree relatives with hyperuricemia and gout are likely to be at risk for developing the condition themselves.
- Medications: There are several medicines that can increase risk for hyperuricemia and gout. These include aspirin (including daily low-dose aspirin for prevention of heart attack and stroke), thiazide diuretics (used for the treatment of high blood pressure, congestive heart failure, including other conditions), immunosuppressant drugs such as cyclosporine (taken after organ transplants and for some rheumatologic conditions), levodopa (Parkinson’s disease), Niacin (used for increasing high-density lipoproteins [HDL] in the blood).
- Alcohol consumption: Moderate to heavy drinking of beer, wine or any liquor increases the risk of hyperuricemia and repeated attacks of gout.
- Exposure to high levels of pesticides and lead is also associated with gout.
- Other health conditions: People with the following conditions have a higher predisposition to gout:
- Obesity
- Diabetes
- High blood pressure
- High cholesterol
- Hypothyroidism
- Kidney disease
- Hematological disorders
What are the complications of uncontrolled hyperuricemia?
If high uric acid levels are not controlled, they can lead to serious chronic medical conditions:
- Chronic gout
- Joint damage and deformity caused by repeated bouts of inflammation and presence of tophi
- Kidney problems
- Hypertension
- Diabetes
- Metabolic syndrome
How is hyperuricemia diagnosed?
Physicians can diagnose gout based on a review of the individual’s medical history, description of symptoms, and a physical exam. The diagnosis will be based on:
- Description of joint pain
- Frequency of experiencing intense pain in joint
- How red or swollen the affected area is
Elevated levels of uric acid can be detected by blood and urine samples. Sometimes, a urine analysis may be repeated after a purine-restricted diet. This can help determine whether the cause of elevated uric acid levels had been because of consumption of purine-rich foods, excessive uric acid production or decreased excretion of uric acid.
If fluid has built up in and around joints, the fluid can be drawn using a fine needle and sent to a lab where it will be examined for presence of uric acid crystals to confirm the diagnosis of gout. Presence of crystals may also be observed on an x-ray of the affected joint.
How is hyperuricemia Treated?
The management of hyperuricemia will depend on the underlying condition. If hyperuricemia is asymptomatic, treatment isn’t recommended. Uric-acid lowering therapies have not been associated with clinical benefit in case of asymptomatic hyperuricemia.
Medications which can prevent or treat GOUT, include:
- Treatment of pain and inflammation:
- Nonsteroidal anti-inflammatory drugs (NSAIDs)
- Colchicine, in case NSAIDs are not tolerated well
- Preventing “attacks” or “flare-ups”:
- Probenecid: Lowers uric acid levels by increasing urination
- Xanthine Oxidase Inhibitors such as allopurinol: Reduce amount of uric acid in bloodstream
The treatment approach for tophaceous gout is the same as for gout, however if the tophi interfere with joint mobility or damage the surrounding tissue, they may need surgical intervention. In rare cases, joint fusion or replacement surgery may be advised.
Treatment of kidney stones
For small kidney stones (<5 mm), physicians may advise the patient to drink a lot of water until the stones pass, and to manage the colicky pain with analgesics. For larger stones, medications may be prescribed to relax the muscles in the urinary tract to make it easier and less painful to pass the stones in the urine. Additionally, a non-invasive procedure known as extracorporeal show wave lithotripsy may be used where ultrasonic energy or shock waves may be used to break the large stone into smaller pieces to facilitate voiding through the urinary tract.
Stones greater than 10 mm in size may need to be extracted with ureteroscopic surgery.
Can certain dietary changes help decrease uric acid levels in blood?
Certain adjustments to dietary regimen may reduce hyperuricemia and the propensity for gout attacks, and may slow progression of joint damage. However, dietary changes should only be an adjunct to the treatment regimen prescribed by the physician, and should not be used as the sole first-line treatment.
Since uric acid is formed when purines break down in the body, avoiding or reducing the consumption of purine-rich foods, may be beneficial in lowering elevated uric acid levels.
Purine-rich foods to avoid or reduce intake:
- red meats (mutton, lamb, pork, beef)
- organ meat (liver, kidney)
- seafood (prawn, crab, lobster, oysters, shrimp)
- oily fish
- beans
- spinach
- peas
- cauliflower asparagus
- lentils
- mushrooms
- oatmeal
- bran
- alcoholic beverages
- yeast supplements
- foods rich in refined sugar (cookies, cakes, pastries)
- sugary beverages (especially those with high fructose-corn syrup)
In addition to reducing intake of purine-rich foods, it is also highly recommended to stay well hydrated and exercise regularly. However, exercise and weight loss strategies should be safe and extreme measures should NOT be adopted. Extreme exercise and weight loss modalities can put additional stress on kidneys, which can impair their ability to excrete uric acid and prevent gout flare-ups.
Dietary modifications and lifestyle changes have been observed to work well for asymptomatic hyperuricemia. Intake of purine-rich food items can be substituted with foods with a low purine-content.
Examples of foods low in purine include:
- Fruits such as pineapple, banana, apples, grapes, raspberries, watermelon, cherries
- Legumes: Soybeans, tofu
- Most nuts and seeds: Cashews, walnuts, flaxseeds
- Whole grains such as oats, brown rice, barley
- Eggs and all dairy products, especially low-fat dairy
- Certain beverages: Coffee, tea, green tea
- All herbs and spices such as chili, cilantro, turmeric
- Plant-based oils including coconut, avocado, olive, flax
- Soup made without meat extract or broth
What is the long-term outlook for individuals with hyperuricemia?
If diagnosed early, most people with hyperuricemia and related symptomatic conditions, i.e., gout and kidney stones can live a normal life.
Compliance with medication, lifestyle, and dietary recommendations can help lower uric acid levels, reduce the frequency and severity of gout attacks, and preserve joint function.