Overview
Head injuries are dangerous and may cause severe medical issues. Subdural hematoma is one of them due to high-impact trauma in the head. It can lead the patient to a coma or even death. This blog is a comprehensive guide on subdural hematoma, its symptoms, causes and treatment options available.
What is a subdural hematoma?
An accumulation of blood outside the brain is known as a subdural hematoma. Blood gathers between the layers of tissue that encircle the brain. The dura is the term for the topmost layer. Bleeding occurs between the dura and the arachnoid, the next layer. It is typically due to severe head injuries and can cause life-threatening bleeding and increased pressure on the brain. Some come to a stop spontaneously, while others require surgical drainage of the accumulated blood.
In subdural hematoma, the bleeding is under the skull and external to the brain. However, when blood collects, the pressure on the brain increases. The symptoms are due to the pressure it causes on the brain. A subdural hematoma can cause unconsciousness and even death if the pressure inside the skull reaches an extreme degree.
What are the different types of subdural hematoma?
Depending on how quickly they form, how much bleeding happens, and how much harm the bleeding causes, doctors categorize subdural hematomas into three different types:
- Acute subdural hematoma: This kind of subdural hematoma is the most hazardous. Severe symptoms appear soon after a brain injury, frequently within minutes to hours. Blood pools and pressure on the brain quickly rises. If one doesn’t get diagnosed and treated right away, they may pass out, become paralyzed, or even die.
- Subacute subdural hematoma: After a head injury, symptoms may show up hours, days, or sometimes weeks later.
- Chronic subdural hematoma: Older adults are more likely to develop this type of hematoma. Slow bleeding can take weeks or months before symptoms show up. Chronic subdural hematomas can result from tiny head injuries. An older adult may not remember how they had a head injury because of the delay in the onset of symptoms. Additionally, the symptoms may go unnoticed by the family because the changes can be extremely subtle and occur slowly.
What are the symptoms of a subdural hematoma?
The rate of bleeding mostly influences subdural hematoma symptoms. After a brain injury, a person may seem normal for a few days and gradually starts losing consciousness. A slower rate of bleeding causes this. Sometimes even after two weeks of bleeding, the symptoms may not appear. But when a subdural hematoma results from sudden, substantial bleeding in a head injury, the victim may immediately lose consciousness or enter a coma.
Subdural hematoma signs and symptoms include a change in behaviour, confusion, dizziness, weakness, lethargy, nausea, diarrhoea, sleepiness, headache or seizures.
These symptoms can vary depending on factors such as age, health issues, and subdural hematoma size, and they can influence how one’s body reacts. Older individuals are more likely to develop slow-growing subdural hematomas. They may cause apathy and subtle personality changes.
Some typical symptoms may include the following:
- Perceptual and constant headaches. In cases of acute subdural hematoma, headaches are generally severe
- Confusion and drowsiness
- Vomiting
- Change in speech and vision
- Lightheadedness, loss of balance, and troubled walking
- Loss of memory, disorientation, and changes in personality, particularly in older adults suffering from subdural hematoma
- Babies with an enlarged head. Soft skulls in babies can enlarge as blood accumulates
The symptoms worsen when the bleeding continues and the pressure builds up in the brain. The symptoms may include:
- Paralysis
- Loss of consciousness and coma
- Breathing issues
When to see a doctor?
If a person experiences these symptoms, immediately visit a healthcare provider and seek help.
What are the causes of subdural hematoma?
Typically, a head injury from a fall, car accident or assault results in a subdural hematoma. The quick blow to the skull breaks blood veins along the brain’s surface. The medical term for this condition is an acute subdural hematoma.
A subdural hematoma is more prone to form in patients who take blood thinners or have a bleeding condition. People who tend to bleed easily may develop a subdural hematoma even after a mild head injury.
Chronic subdural hematoma is more common in older individuals due to brain shrinkage, making the tiny veins more strained and prone to ripping.
Who is at risk of developing subdural hematoma?
Anyone can experience a subdural hematoma due to head trauma, but certain people are more susceptible to subdural hematoma. It is common among the following people:
- Older adults: As a person ages, the brains shrink within the skull, causing a large gap between the skull and the brain. The large gap enables the tiny veins in the membrane between the skull and the brain to stretch. Eventually, the stretched and thinned vein will most likely tear in a minor head injury, including a fall from a chair.
- Contact sportsperson: Sports players involved in high-impact sports like football are at a greater risk of developing a subdural hematoma.
- People taking blood thinners: Blood thinners medications decrease the clotting process or prevent the blood from clot completely. When the blood fails to clot, it causes severe and long-lasting bleeding after a minor injury.
- Haemophiliacs: People who have haemophilia are known as haemophiliacs. Haemophilia is a genetic disorder that stops the blood from clotting. Patients with haemophilia are at a higher risk of uncontrolled bleeding after any injury.
- Alcoholics and people with alcohol use disorder: Over time, excessive drinking leads to liver damage. A damaged liver fails to produce proteins sufficient proteins that assists blood in clotting. Thus, increasing the risk of uncontrolled bleeding.
- Babies: Babies lack strong neck muscles to protect themselves from trauma to the head. Therefore, when a person vigorously shakes a baby, they can develop a subdural hematoma. Such an injury is called shaken baby syndrome.
What measures are used to diagnose subdural hematoma?
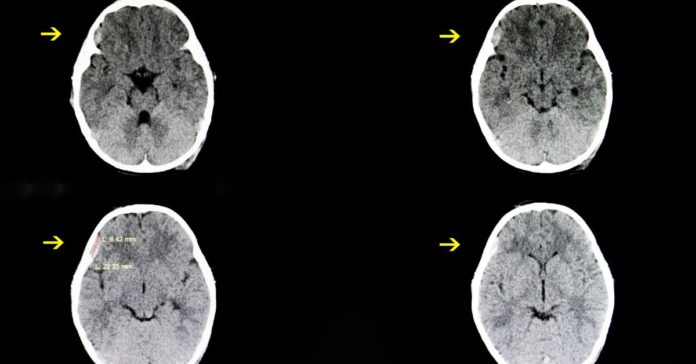
Following a head injury, patients frequently have their heads imaged, typically through a computed tomography (CT) scan or magnetic resonance imaging (MRI scan). These exams produce images of the skull’s interior and typically identify any subdural hematomas. Although CT is quicker and more accessible, MRI detects subdural hematomas more effectively. Angiography may very seldom be utilized to identify a subdural hematoma.
What are the treatment options for subdural hematomas?
The severity of subdural hematomas determines the treatment options. The only recommended course of action for minor subdural hematomas with moderate symptoms is to stay under observation. It is common practice to do repeated head imaging to check on the progress of the subdural hematoma.
Surgery is necessary to relieve the pressure on the brain in more severe or acute subdural hematoma cases. Doctors use different surgical procedures to treat subdural hematomas:
- Burr hole trephination: A hole is bored into the skull above the site of the subdural hematoma. It helps in suctioning excessive blood.
- Craniotomy: In this procedure, doctors remove a considerable portion of the skull to relieve pressure. Once the pressure is reduced, the excised skull is replaced.
- Craniectomy: Here, the doctor removes a portion of the skull for an extended time. The procedure assists the wounded brain in enlarging and expanding without suffering long-term damage. Subdural hematoma is not often treated with a craniectomy.
Serious illness necessitates the use of machines to maintain breathing and other forms of life support in patients with severe subdural hematomas. Improvements in blood coagulation should be made if a person has a bleeding issue or is taking blood thinners. This can entail administering medications or blood products and, if possible, stopping any blood thinners. Additional medicines may also be needed to help manage seizures or relieve lower brain pressure or swelling.
What are the complications of subdural hematoma?
Severe consequences from some subdural hematomas may result in coma or even death. It may occur if the hematoma is left untreated. Potential issues include:
- Herniation of the brain: Subdural hematoma will make the brain push tissue out of its normal position. Death may result from this.
- Bleeding: During the healing phase of the initial haemorrhage, older people are more likely to experience additional bleeds, particularly if they have suffered head injuries.
- Seizures: Despite having the hematoma repaired, the patient may still experience seizures.
Conclusion
Subdural hematoma is a dangerous condition that can be fatal. Depending on the patient’s age, the severity of the head injury, and how promptly they received care, the prognosis for health following a subdural hematoma can vary. The chances of surviving are higher among the younger ones. After a subdural hematoma, older persons are more at risk of experiencing another brain haemorrhage. So, seek the proper medical help at the right time.
Frequently Asked Questions (FAQs)
What are the ways to prevent subdural hematoma?
Prevention is better than cure. So, follow ways to protect the head from injuries, such as wearing a seat belt and helmet while riding vehicles. Remember to use protective gear while playing high-impact contact sports. Make sure to avoid surfaces that make elders slip.
Who is at more risk of getting subdural hematoma?
Older adults, babies, people who take blood-thinning medications, athletes, and people with haemophilia are more at risk of getting subdural hematoma.
Can medications cure subdural hematoma?
In some non-severe cases, medications may cure subdural hematoma.