Overview:
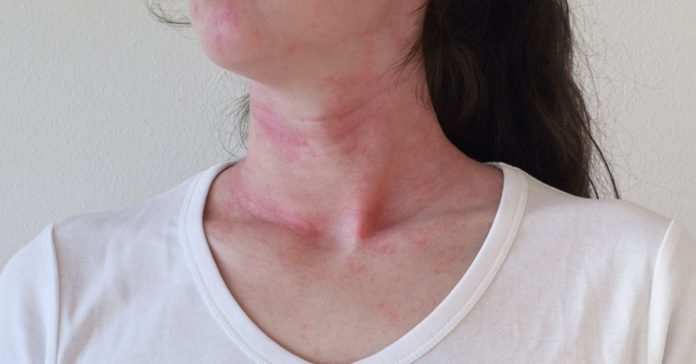
Systemic capillary leak syndrome, also referred to as Clarkson’s disease, is a condition wherein your plasma from the blood leaks into adjacent body muscles and cavities that in turn may lead to a sharp drop in blood pressure that may lead to organ failure, or even death. Although it is a life-threatening situation, early identification and timely intervention can reduce the mortality rate.
About Systemic Capillary Leak Syndrome (SCLS)
Systemic capillary leak syndrome or SCLS is often confused with anaphylactic shock, septic shock, and polycythemia. However, it is different as it gets triggered by either physical exertion or the upper respiratory tract infection. The intensity and duration of this syndrome vary to a great extent. It can attack either once in a lifetime or occur several times in a year.
What are the symptoms of systemic capillary leak syndrome?
Systemic capillary leak syndrome manifests after an initial couple of days after non-specific symptoms like:
This is followed by a leakage of plasma from blood vessels into body cavities leading to sudden drop in blood pressure and organ damage .
When to see a doctor?
If you observe any of the abovementioned symptoms, contact your doctor to diagnose your health condition. Also, visit your doctor in the following cases:
- Low blood pressure.
- Increasing body weight without any reason.
- Continuous muscle pain that doesn’t subside.
- Edema: It is a condition where your body parts become swollen because of excessive accumulating fluid
Request an appointment at Apollo Hospital
Call 1806-500-1066 to book an appointment.
What are the causes of systemic capillary leak syndrome?
While the cause of systemic capillary leak syndrome (SCLS) is not yet known, there looks to be no hereditary predisposition for this condition. More than half of SCLS patients have a M protein or monoclonal detected in their blood. Usually, the level of M protein, produced by plasma cells in the marrow, is low.
The role of M protein in acute attacks is still not known There are numerious possible explanations for production of M protein in patients with SCLS including an autoimmune mechanism where our own immune system mistakenly attacks the body. Lately it has been said that capillary lining cells may get damaged by a factor in our blood which is produced during an acute attack.
Treatment for systemic capillary leak syndrome
The first phase of treatment that often lasts many days, is known as the resuscitation phase, which is aimed at controlling capillary leaks and maintaining blood pressure. In that phase, Intravenous fluid replacement is usually required, but should be minimized due to its propensity to leak into tissues.
Excess intravenous fluid administration that could result in massive swelling of the extremities requiring surgical decompression. Measurement of arterial pressure or central venous in an intensive care unit is often needed to achieve a delicate balance. Intravenous albumin and colloid may be used. Glucocorticoids (steroids) are used often during an acute attack, particularly early in the recruitment phase.
In the second phase, sometimes called the recruitment phase, diuretics may be needed for excess fluid overload.
In an attempt to decrease the frequency and severity of acute attacks, maintenance therapy is offered. The current standard of care for systemic capillary leak syndrome is administrating immunoglobulins intravenously once a month for an indefinite period of time.
Secondary medicines may include a combination of terbutaline and theophylline. Leukotriene inhibitors like montelukast or an ACE inhibitor like lisinopril may be beneficial.
Conclusion
Systemic capillary leakage disorder is diagnosed with three factors- low protein levels in your blood, low blood pressure, and increased hematocrit. However, these factors alone do not indicate Clarkson’s disease.
Frequently Asked Questions (FAQs)
Is Clarkson’s disease fatal?
In case of medical negligence or absence of timely medical intervention, Clarkson’s disease may turn out to be fatal, even leading to the death of the patient.
How is Clarkson’s disease diagnosed?
Clarkson’s disease gets concluded after numerous diagnostic tests, including physical examination, recurrence of symptoms, and other laboratory tests. Hematocrit tests, levels of hemoglobin, and M protein also get checked to diagnose the condition.