Overview
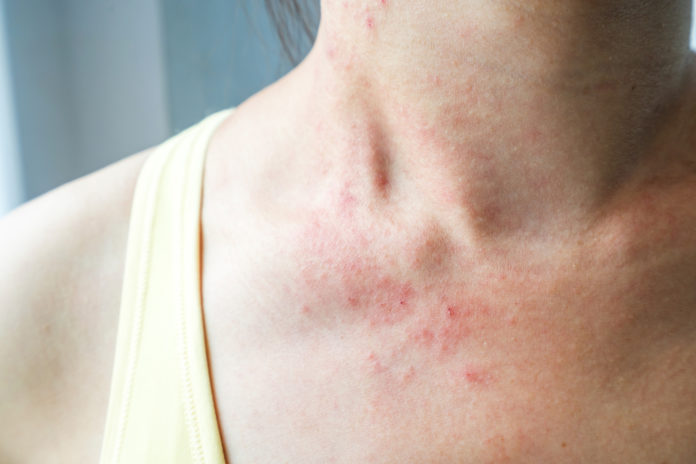
Sweet syndrome causes fever with painful skin rash, mostly on the face, neck, and arms. Sweet syndrome is an unknown skin condition called acute febrile neutrophilic dermatitis. However, the exact cause of Sweet syndrome is unknown; but can be triggered due to medication, illness, and infection. Additionally, Sweet syndrome can also occur along with some type of cancer. Sweet syndrome as a disease is not contagious, not a form of skin cancer, and is not hereditary. Sweet syndrome is generally treated with corticosteroids.
What are the Signs and Symptoms of Sweet Syndrome?
Sweet syndrome signs and symptoms can vanish after treatment in a few days but can come back again. Some of the common symptoms of Sweet syndrome are as follows:
- Fever
- Bumps that grow easily in size and spread into painful clusters.
- Small painful red bumps on back, neck, face, and arms.
- Muscle and joint pain
- Skin and mouth lesions
- Skin discoloration
- The feeling of being unwell.
Thus, if you witness any of the symptoms mentioned above or develop a painful red rash that grows quickly in size, you should immediately get in touch with the doctor to decide on the treatment plan.
Call 1860-500-1066 to book an appointment
How Does Sweet Syndrome affect the Skin?
The most common changes in the skin in Sweet syndrome are the development of red-to-purple tender skin patches or lumps that can be small or large or can join together to form a larger lump. Additionally, pustules and blisters can be seen, and the rash appears at the site of injury and can lead to infection.
Sweet syndrome affects other internal organs and tissues in addition to the skin. The other body parts that are affected due to Sweet syndrome are bones and joints. Additionally, ears, eyes, and mouth are also affected by Sweet syndrome. The red bumps can extend from the external ear to the eardrum. Eyes can get swollen with redness and inflammation. Sweet syndrome can cause sores on the tongue, inside cheeks, and gums. Also, it is observed that inflammation of the internal organs of the chest and abdomen can happen due to Sweet syndrome.
What Causes Sweet Syndrome?
The exact cause of Sweet syndrome is unknown. However, sometimes the condition is associated with some types of cancers such as blood cancer, breast cancer, colon cancer, etc. Additionally, Sweet syndrome can also occur due to a medication reaction that boosts white blood cell production in the body.
How is Sweet Syndrome Classified?
The doctors classify Sweet syndrome in three categories, which are as follows:
- Malignancy-associated Sweet Syndrome. It appears in certain types of cancer, such as acute myeloid leukemia.
- Classical Sweet Syndrome. Sweet syndrome can also occur with other medical conditions such as upper respiratory infections, gastrointestinal infections, and pregnancy.
- Drug-induced Sweet Syndrome. Sweet syndrome can be triggered by some medications, such as sulfamethoxazole and trimethoprim, granulocyte colony-stimulating factor (G-CSF), and NSAIDs.
What are the Risk Factors Associated with Sweet Syndrome?
Sweet syndrome is a rare disease, but some factors would increase your risk of being diagnosed with the disease are as follows:
- Age. Sweet syndrome can occur at any age. However, the disease mainly affects people aged between 30 years to 60 years.
- Sex. It is observed that women are more prone to be diagnosed with Sweet syndrome compared to men.
- Cancer. Sometimes, Sweet syndrome is associated with cancer such as leukemia, breast, or colon cancer.
- Pregnancy. Some women may be diagnosed with Sweet syndrome during pregnancy.
- Drug sensitivity. Sweet syndrome can also result from sensitivity towards few drugs such as azathioprine and some non-steroidal anti-inflammatory drugs.
How is Sweet Syndrome Diagnosed?
A dermatologist would diagnose Sweet syndrome by physical examination of your skin. However, to better diagnose and assess Sweet syndrome, the healthcare professional would prescribe a few tests, which are as follows:
- Skin Biopsy. The doctor would remove a small piece of the affected tissue for examination.
- Blood Tests. The blood sample is sent to the laboratory to check the count of white blood cells and other blood parameters.
How is Sweet Syndrome Treated?
Sweet syndrome can sometimes disappear without any treatment, but the recovery process can be speeded up by using medications. The most common medications prescribed for the treatment of Sweet syndrome are as follows:
- Oral Treatments. Oral corticosteroids work well for the treatment of Sweet syndrome. However, long-term use of these pills can lead to side effects such as insomnia, weakened bones, and weight gain.
- Steroid tablets such as prednisolone are effective for the treatment of Sweet syndrome.
- Immunosuppressive agents such as cyclosporine can be useful for the treatment of Sweet syndrome.
- Other medications, such as daps one, potassium iodide, colchicine, and indomethacin, can help treat Sweet syndrome.
- Injections. Injecting a small amount of corticosteroid into the lesion can be done.
- Ointments and Creams. These are applied to the skin’s affected area, but they can cause skin thinning.
The healthcare professional would prescribe the medications mentioned above for several weeks to avoid relapse. Some of the alternative medications that the doctor can prescribe if consumption of corticosteroid in the long-term is a problem:
- Colchicine
- Potassium iodide
- Dapsone
Conclusion
If you have had a fever for the past few days, a bumpy rash all over your body, and it is spreading fast, and those rashes are hurting, it would need medical attention. Sweet syndrome is not contagious, nor is it a form of skin cancer or hereditary. It can be vanish sometimes without any medications; however, taking medication can speed up the recovery process. It has been observed that Sweet syndrome can revert even after treatment. Some of the medications prescribed by healthcare professionals to treat Sweet syndrome are steroids, immunosuppressive agents, and other medications. Few of these medications can have certain side-effects, and your dermatologist may advise regular blood tests to monitor the prescribed treatment.