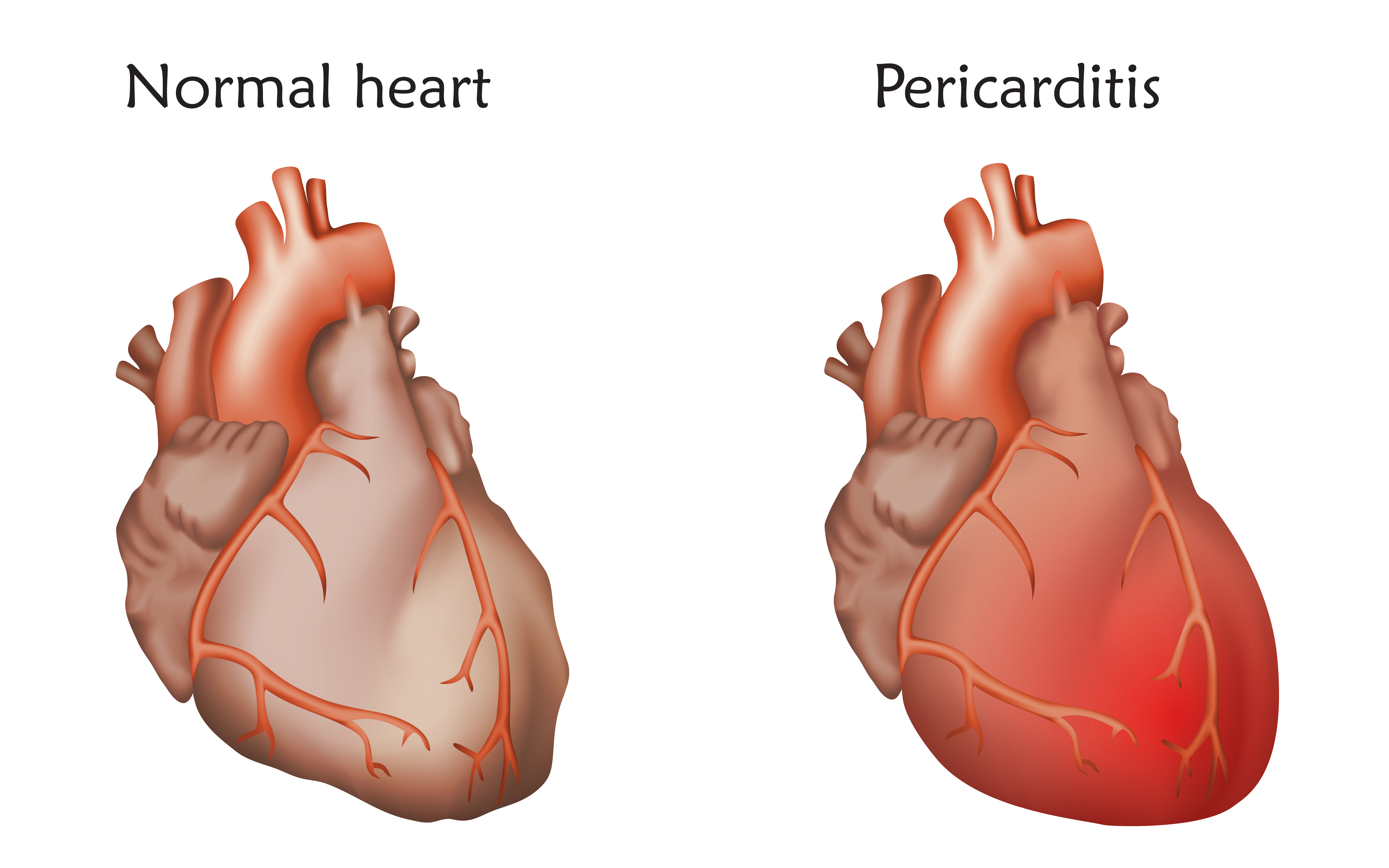
Pericarditis is an inflammation of pericardium. This is a disease that can develop suddenly and can last for several months. The pericardium is a thin and two-layered sac filled with fluid, covering the outer area of your heart. This provides lubrication—acting as a shield for the heart to protect it.
What is Pericarditis?
Pericarditis can be attributed to several factors, including viral, bacterial, fungal and other infections. Other possible causes of pericarditis include heart attack or heart surgery, other medical conditions, injuries and medications. Pericarditis can be acute, meaning it happens suddenly and typically doesn’t last long. Or the condition may be “chronic,” meaning that it develops over time and may take longer to treat. Both types of pericarditis can disrupt your heart’s normal rhythm or function. In rare cases, pericarditis can have very serious consequences, even leading to death. Most of the time, pericarditis is mild and clears up on its own with rest or simple treatment. Sometimes, more intense treatment is needed to prevent complications.
What are the Types of Pericarditis?
There are several stages of pericarditis, and each one of them is identified by different symptoms.
- Acute pericarditis: This type of pericarditis starts suddenly, but patients are likely to observe pain and other signs for two to three weeks. However, the possibility of it occurring again is likely. It can be difficult to evaluate the difference between the pain because of a heart attack and acute pericarditis.
- Recurrent pericarditis: After you have faced an episode of acute pericarditis, there is a possibility of recurrent pericarditis. It occurs about four to six weeks after you have suffered from acute pericarditis, and you are likely to observe any symptoms in between the time frame.
- Incessant pericarditis: This type lasts from four to six weeks and does not last more than three months. You can observe continuous symptoms like chest pain.
- Chronic constrictive pericarditis: This is a type as it develops slowly and has a longer duration than incessant pericarditis, like more than three months.
What Symptoms Show That a Person is Suffering from Pericarditis?
- Chronic chest pain: It is one of the common symptoms of acute pericarditis where the person might suffer severe, stabbing, sharp, and sudden chest pain. Often this pain is observed at the left side or middle side of the chest.
- Severe pain behind the breastbone: It comes as a quick pain at the left side of your chest, making you feel extremely uncomfortable. The pain gets worse while coughing or lying down.
- Pain in the left shoulder and neck: The same kind of pain occurs during heart attacks, so most of the time, it can be confusing. But the difference is that in pericarditis, the pain is sudden and sharp, which goes through your left shoulder to neck and then reaches the back.
- Excessive pain while coughing or sleeping: The chest pain gets worse and sharp, which can create problems of excessive pain to an individual while coughing or lying down.
- Swelling in the abdomen or legs: People suffering from chronic pericarditis can have swelling in the abdomen & legs
- Cough or shortness of breath: Person might feel shortness of breath.
- Fatigue or weakness: Chronic pericarditis can cause scarring of the pericardium, which makes it difficult for the heart to perform its main function, making the person extremely tired and weak.
- Low-grade fever
- Heart palpitations (increase in a heartbeat)
- Pericardial effusion: It is the symptom when the fluid builds-up in the pericardium, making it difficult for your heart to function
When is the Right Time for a Medical Consultation?
If you notice severe chest pain or pain around your left shoulder and arms, you need to consult a doctor immediately. Several pericarditis’ symptoms are similar to a heart attack , so it is essential to evaluate what is causing you the trouble. The sooner it is done, the faster you are pain-free.
Call 1860-500-1066 to book an appointment
What are the Causes of Pericarditis?
The causes behind pericarditis are hard to identify, but during the diagnosis, the doctor can evaluate causes like:
- Heart attack
- Heart surgery
- Infection
- Systemic inflammatory disorders
- Trauma
- Accident causing injury to the heart
- Health disorders
- Viral or bacterial pericarditis
- Autoimmune diseases
- Fungi and parasites
- Pericardium tumors
- Radiation therapy
- Genetic disease
- Metabolic disorders
What are the Risk Factors Associated with Pericarditis?
- Recovery from a heart attack
- Genetic disorders
- Autoimmune diseases
- Some bacterial, viral, and fungal infections
- Renal failure
- Certain medications
What is the Treatment for Pericarditis?
Depending on the severity of your problem, the treatment process is followed. If you are suffering from mild pericarditis, then with proper treatment, you can recover really fast.
Medications: Oral medications are the first approach, which is done to relieve the pain by giving pain-killers. Mostly OTC pain relievers are prescribed. Some other medications are given that helps to reduce the inflammation to treat pericarditis.
Surgery: If there is fluid build-up because of pericarditis around the heart, the doctors will first drain out that extra fluid to resolve the functioning of your heart. The surgery can be:
- Pericardiocentesis, where the doctor uses a catheter to drain the excess fluid build-up from the pericardial cavity.
- Pericardiectomy, where the doctor removes the entire pericardium. This surgery is initiated when the fluid-filled sac becomes perpetually stiff because of chronic constrictive pericarditis.
Recovery from pericarditis may take a few days to weeks or even months. Sometimes there is an extra fluid secreted between the pericardial layers; this problem is known as pericardial effusion. There is no specific age risk factor, as pericarditis can happen to anyone of any age group.
What Complications Can Occur with Pericarditis?
If diagnosed and treated earlier, the risk and complication generally decrease. Still, other complications that patients have to face are:
Pericardial effusion: In this situation, when the fluid build-up is extreme around the heart, it can put extended pressure around it, making it difficult for the heart to pump.
Chronic constrictive pericarditis: In this case, there can be permanent stiffening and scarring of the pericardium, making it difficult for the heart to pump. It also leads to an excessive abdomen and leg swelling, along with shortness of breath.
Cardiac tamponade: Here, excessive fluid is collected in the pericardium. This extra fluid puts extreme pressure on the heart, preventing it from filling up the blood. This lack of blood causes a drop in blood pressure, leading to cardiac tamponade. Patients with this complication require emergency treatment.
What are the Preventive Measures for Pericarditis?
It is difficult to prevent acute pericarditis. But, with proper treatment and medication, you can prevent future episodes of acute pericarditis or other types of pericarditis. In order to protect yourself from forthcoming episodes, you need to consult your doctor
Conclusion
Pericarditis can go away within a short span of time. But, it is important to get it diagnosed by an experienced medical professional so that you can get the right treatment plan to treat it.
With proper rest and care, you can recover in a short time and live normally.
FAQs
What are the main causes of pericarditis?
The general cause behind this illness is still unknown. However, the common indicator for pericarditis is viral infections, especially some respiratory infections. Chronic and recurrent pericarditis can be caused because of immune system disorders.
Is pericarditis condition an emergency situation?
Acute pericarditis can be treated with medications. But, if there is fluid build-up around the heart, making it difficult to operate, then it is considered an emergency situation, where doctors will prepare you for the surgery to drain out the fluid and get your heart back to pumping blood.
Can pericarditis cause damage to the heart?
If the fluid build-up is extreme in the sac or around the pericardium, it can drastically affect the heart. When the fluid is filled up, it becomes difficult for the heart to fill up or draw out the blood, which puts pressure, preventing it from pumping accurately. This also decreases blood pressure, making it life-threatening.